Easy Telemedicine for Azalea Health | One Tap to See Your Doctor
💡 Easy telemedicine for Azalea Health rural patients works through text-based video visits that require no app, no account, and no download. ...
11 min read
Aubreigh Lee Daculug
:
March 20, 2026

The phone rings at 7:30 AM. "I can't make it in today — my truck won't start." And just like that, your 10:00 AM slot is gone.
For rural clinics on Azalea Health, that call is a familiar one. Patients want to come in. They know they need to. But distance, weather, and transportation make it harder than it should be.
The result? Empty slots, idle providers, and care that keeps getting pushed back.
Azalea Health staff text-based telemedicine to reduce no-shows at rural clinics is no longer a workaround — it's a real, proven strategy.
Curogram integrates directly with Azalea Health, giving front desk staff at Rural Health Clinics (RHCs), Federally Qualified Health Centers (FQHCs), and Critical Access Hospitals a simple way to respond to every cancellation call: offer a video visit instead.
The script is one sentence:
"We'll text you a link at your appointment time. Just tap it and you'll see the doctor from your phone."
No app to download. No portal to log into. No tech support needed.
The patient gets their care. The provider stays busy. The slot that was about to go empty becomes a completed visit.
Rural clinic front desk staff are often the first — and only — line of defense against a no-show. When they have the right tool, they become visit-savers instead of cancellation-takers. That's exactly what Curogram is built to do.
This article walks through how the workflow works, why it fits the rural healthcare context, and what it means in practice for office managers and front desk teams running busy schedules on Azalea Health.
Every open slot at a rural clinic is a direct hit to the bottom line. A provider seeing 20 to 25 patients per day at a Critical Access Hospital only needs two or three cancellations to feel it — and over weeks and months, those lost visits add up to real money.
Unlike larger urban practices that may have waitlists long enough to fill same-day gaps, most rural clinics simply don't have that cushion.
The next patient on the schedule often lives 40 or 50 minutes away. Calling them to come in on two hours' notice isn't a realistic option. So the slot stays empty, the provider sits idle, and the revenue is gone.
What makes this especially frustrating is that the cancellation wasn't the patient's fault, and it wasn't yours either. It's simply the reality of practicing medicine in a rural community.
The drive that's manageable on a clear Tuesday morning becomes impossible when the roads are icy or the car won't start. And unlike a missed appointment in an urban clinic, there's no one nearby to fill the gap.
When cancellations stack up — even just two or three per week — the cumulative effect is significant, especially without mass texting workflows that can instantly redirect patients to virtual visits during weather disruptions.
Multiply those lost slots over a quarter, and the revenue picture starts to look very different from what the schedule promised at the start of each month.
Behind every empty slot is a patient who actually needed that visit.
Think about what gets postponed when a cancellation doesn't get recovered:
When a visit gets rescheduled instead of recovered, the gap stretches from days to weeks. And by the time that new date arrives, the same transportation barrier may cancel it again.
For patients managing chronic conditions, that cycle is genuinely dangerous — especially given how telehealth helps maintain continuity of care for chronic disease management.
The rescheduling spiral is harder to see than a revenue gap, but it's just as real. A patient who cancels three times in a row isn't being negligent — they're facing the same structural barriers every single time.
Without a path around those barriers, their conditions quietly worsen between visits, and the clinic loses the chance to intervene when it matters most.
This is one of the most under-discussed consequences of rural no-shows. The financial impact shows up on a report. The care gap doesn't — until a patient comes in months later with a condition that's progressed further than it should have.
Front desk staff at rural clinics hear the same handful of reasons every week: can't get a ride, roads are bad, truck broke down, can't take time off work, kids are home sick.
These aren't excuses — they're the real logistics of rural life. The patient wants to come in. They know they should. Without a virtual alternative, geography wins every time.
That's the reality for most office managers handling a rural clinic front desk telemedicine workflow on Azalea Health.
The staff member who picks up that call isn't frustrated with the patient — they're frustrated with the situation. There's nothing to offer but a new date on the calendar, and everyone on both ends of the line knows that date is just as uncertain as the one that just fell through.
That helplessness is what Curogram is designed to replace.
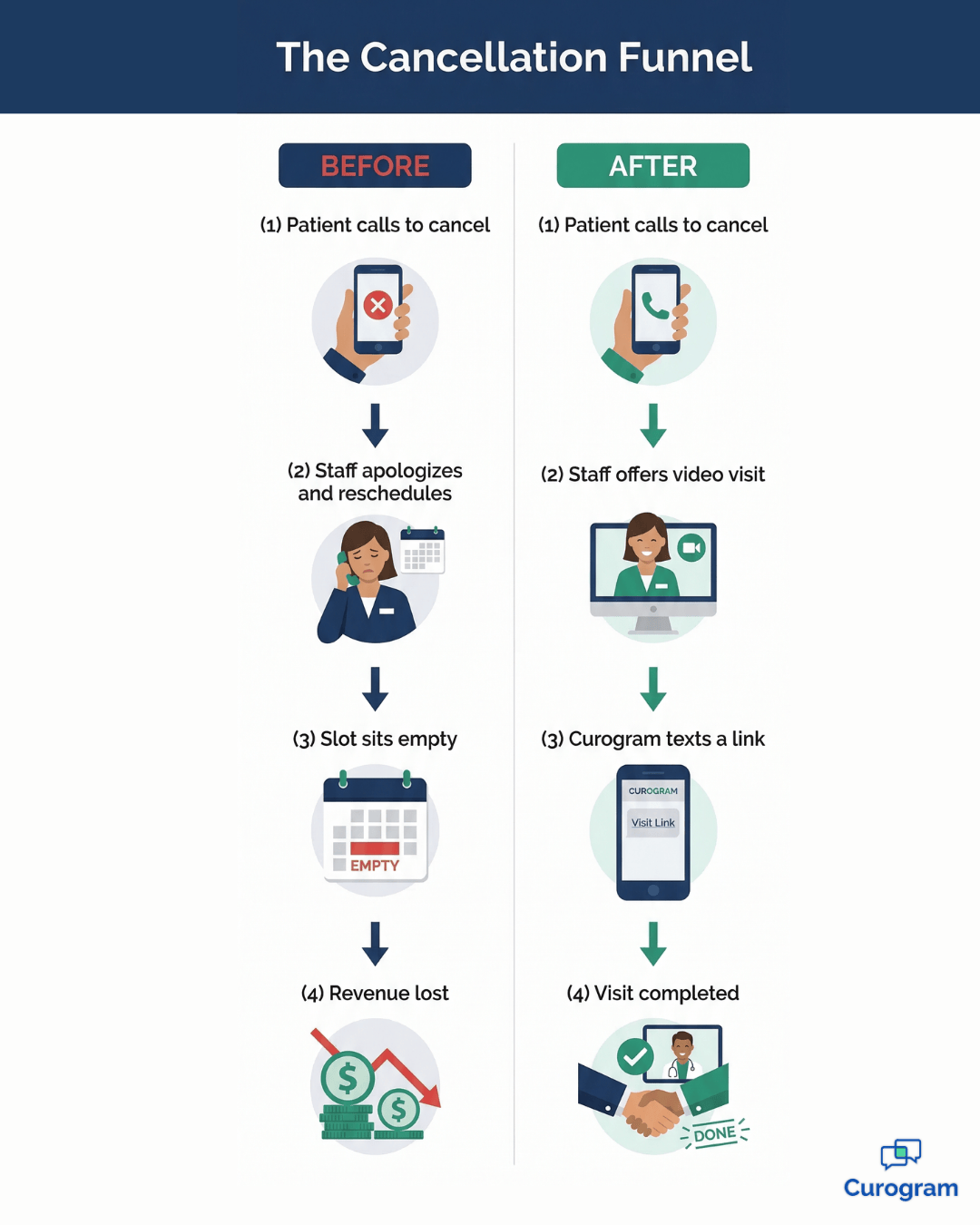
Curogram gives front desk staff a different response when a patient calls to cancel. Instead of apologizing and offering to reschedule.
They can say:
"We can do that as a video visit instead. We'll text you a link at your appointment time — just tap it and you'll see the doctor from your phone."
That one sentence changes the outcome entirely. The visit doesn't get lost. The provider stays on schedule. The patient gets their care without having to find a ride or brave bad roads.
What makes this response so effective is how easy it is for the patient to say yes — especially when appointment reminder texts already include the video visit link patients need to join instantly.
There's no setup, no tech learning curve, and no new obligation. They're already on the phone.
They already had that time blocked off. All they have to do now is stay home and wait for a text — which is a far easier ask than rearranging transportation and taking time off work.
For front desk teams who've spent years hearing the same cancellation stories, this is a genuine relief. Instead of ending calls with a rescheduled date that everyone suspects might fall through again, they end them with a plan that actually works.
The conversion process fits the way front desk staff already work — there's no new system to learn.
Here's the full sequence from cancellation call to completed visit:
Documentation flows back to the patient chart just like any other visit. The reduce empty appointment slots telehealth text message approach is exactly this straightforward — no separate software to open, no extra logins for staff.
The speed of the conversion is worth noting. A staff member who knows the workflow can complete it in under two minutes while still on the phone with the patient. By the time the call ends, the appointment is already converted, the text is queued, and the slot is saved.
There's no follow-up action required — the system handles the rest automatically.
One of the biggest friction points with telemedicine at smaller practices is the platform-switching problem. Staff log into one system to manage the schedule and a completely different one to launch the virtual visit.
That's two logins, two workflows, and twice the chance for something to go wrong mid-day.
Curogram eliminates that through its direct integration with Azalea Health. Virtual visits appear on the provider's schedule alongside in-person appointments, and the team never has to leave the system they're already in.
For a rural clinic front desk telehealth workflow on Azalea Health, that kind of seamless experience is what actually gets adopted — and stays adopted.
This matters more than it might seem. Telemedicine tools that require staff to switch platforms often get abandoned after the first few weeks — not because the technology is bad, but because the extra steps create enough friction that staff default to the path of least resistance.
When telemedicine lives inside the workflow people already use, it becomes habit instead of a workaround.
Providers feel the difference too. They don't have to launch a separate application or log into a different portal between patients.
The video visit is right there on their schedule, next to the in-person appointment that follows it. It's a smoother day — and smoother days mean providers can stay focused on care rather than technology.
Most telemedicine platforms assume a patient who's comfortable downloading apps and creating accounts.
That's not always who's sitting on the other end of a cancellation call at a rural health clinic or FQHC. Curogram's staff-initiated telemedicine text link works differently. The patient gets a standard SMS at their appointment time, taps it, and they're in.
Nothing to install. No account required. If a patient can read a text message, they can join the visit.
This is especially important for older patients and those with limited experience navigating smartphones.
A traditional telemedicine platform might ask them to download an app, create a username, verify an email, and then find and tap a join button — all steps that can derail a visit before it even starts. Curogram removes every one of those steps. The link in the text is the entire process.
Practices that have tried other telemedicine solutions often cite patient drop-off at the setup stage as their biggest obstacle. Patients agree to the video visit, then can't figure out how to join and give up. That failure doesn't happen with a one-tap link delivered by standard text.
It works on any phone, with any carrier, and requires no preparation on the patient's end whatsoever.

Based on our internal data, practices using Curogram's text-based telemedicine see no-show rates drop by up to 53% compared to the industry average.
Each converted visit means a provider who stays productive, a patient who gets care on time, and revenue that doesn't disappear into an empty slot.
For smaller rural practices, even a 10 to 20% increase in monthly visit volume can meaningfully improve the bottom line.
Based on our internal research, each recovered appointment contributes directly to profitability. Fewer empty slots means more revenue — it's a straightforward equation, and it compounds over a full season of winter cancellations.
The impact is most visible at practices with high cancellation rates during specific seasons or weather patterns. A clinic that previously lost a dozen visits every winter month to transportation-related cancellations can recover the majority of those slots once staff have the tool to offer a virtual alternative.
Over a full winter season, the difference in revenue is substantial.
It's also worth considering what else improves alongside the numbers. Provider utilization goes up. Patient satisfaction improves because people are getting care instead of being pushed back on the calendar.
And staff morale gets a quiet boost when the frustrating routine of fielding dead-end cancellation calls is replaced by something more productive.
The shift that happens at the front desk is just as important as the revenue numbers. When staff have a clear, easy alternative to offer every cancelling patient, the way they handle those calls changes entirely. It stops being a dead end and starts being an opportunity.
Office managers at Critical Access Hospitals and FQHCs who have implemented this workflow describe the same change in team confidence.
The convert cancellations to virtual visits FQHC model also helps with care continuity in a way that traditional rescheduling never can — patients who would have waited three to four weeks get their visit on the original day, on the original schedule.
Their chronic conditions don't drift. Their care plans stay on track.
There's also a longer-term effect on patient retention. When patients know that a transportation problem won't mean losing access to care, they're more likely to stay engaged with their clinic.
They don't drift toward another provider or simply stop scheduling follow-ups. The relationship holds, and the clinic keeps the patient.
That kind of continuity is hard to quantify but easy to feel in a practice that's been using the tool through a full year.
Staff who go through this shift often describe a change in how they think about their own role. They're not just administrative gatekeepers for the schedule — they're actively participating in keeping patients connected to care.
That's a meaningful difference, and it tends to show up in how they communicate with patients across every call, not just cancellations.
Consider a front desk coordinator at a two-provider rural health clinic on Azalea Health. In winter months, she used to field four to six cancellation calls per day — nearly all due to weather or transportation.
Each one was a lost visit and a patient whose care was delayed.
After implementing Curogram's text-link telemedicine, she began offering a virtual alternative to every cancellation. Her conversion rate averaged around 60%: of the patients who called to cancel, more than half agreed to a video visit when told a link would be texted to them.
In her first winter with Curogram, the clinic recovered dozens of visits that would otherwise have been no-shows.
What's notable about that 60% rate is what it represents in practice. For every ten patients who called to cancel, six of them ended up getting their care that same day — at the same time they originally scheduled.
Their providers stayed busy. The clinic kept the revenue. And the patients who'd been managing chronic conditions didn't have to wait another few weeks just because their truck wouldn't start.
Her words say it best: "Now when someone calls to cancel, I don't feel helpless. I have something to offer them."
Every cancellation call is a fork in the road. Down one path, you apologize, reschedule, and watch the slot go empty. Down the other, you offer a video visit, the patient taps a link, and the visit happens anyway.
Curogram puts your front desk team on the second path — every time.
The office manager telemedicine scheduling tool for Critical Access Hospitals and rural practices doesn't have to be complicated. It doesn't have to require a separate platform, a new login, or a week of staff training.
With Curogram's integration on Azalea Health, the workflow is the same one your team already knows — the only change is that cancellations now have a better answer.
Azalea Health handles your scheduling and clinical documentation. Curogram handles patient access when they can't walk through the door. Together, they make sure a cancelled drive doesn't have to mean a cancelled visit.
Your providers stay productive. Your patients stay in care. Your revenue doesn't disappear every time the weather turns.
The front desk staff who hear those early-morning cancellation calls are often the deciding factor between a lost visit and a completed one. Give them the tool to make the better call — every single time. One successful conversion will change how your team thinks about cancellations forever.
Ready to see how it works? Schedule a demo today and start converting cancellations into virtual visits. Your next no-show doesn't have to be a no-show at all.
Very little. The workflow for staff is simply to switch the in-person appointment to a virtual visit inside Azalea Health. Curogram sends the patient a text at appointment time with a direct video link — no separate telemedicine platform to log into, no new process to memorize. The patient-facing script is one sentence. Most front desk teams are comfortable offering virtual visits after their first day.
Curogram can send an automated reminder text a few minutes before the visit to prompt the patient. If the patient still hasn't joined within a couple of minutes of the scheduled time, staff can send a follow-up text or place a quick call to check in. In practice, the tap-to-join simplicity means most patients connect on time. It's significantly easier for a rural patient than navigating a traditional app-based telemedicine platform.
Yes. Because Curogram integrates directly with Azalea Health's scheduling system, virtual and in-person visits appear side by side on the same calendar. A provider can see a patient in person at 9:00 AM, join a video visit at 9:30 AM, and return to in-person at 10:00 AM — all without switching platforms. The video visit launches from the provider's workstation with a single click.
Yes. Curogram is a fully HIPAA-compliant platform. The video link sent via text uses a secure, encrypted connection. No protected health information is transmitted through the text message itself — the link simply opens the secure video session. Practices can use the platform confidently knowing that patient privacy is protected at every step.
That's one of the main reasons rural clinics choose Curogram. There's nothing to download, nothing to install, and no account to create. The patient receives a standard text message and taps a link — that's the entire process. If a patient can use a smartphone to read a text message, they can join a Curogram video visit. It removes the tech barrier that stops many rural patients from using other telemedicine platforms.

💡 Easy telemedicine for Azalea Health rural patients works through text-based video visits that require no app, no account, and no download. ...

💡 eClinicalWorks telemedicine with zero-download, browser-based video visits lets enterprise networks launch virtual appointments directly from the...

💡 To launch telehealth Meditab IMS practice no IT requirements no app downloads, send patients a text link they tap to open a browser-based video...