eCW Billing Text-to-Pay | Cut Statement Costs & Automate Posting
💡 eClinicalWorks billing teams spend a large part of their time managing paper statements, chasing balances, and posting payments by hand. This...
8 min read
Jo Galvez
:
Updated on April 12, 2026

A patient visits their doctor on Monday. By Thursday, a paper bill is in the mail. By the time it lands on the kitchen counter, the visit feels like a distant memory.
That gap, between care and payment, is where revenue disappears. For enterprise eClinicalWorks networks managing dozens of providers across many sites, that gap can cost millions each year.
The problem isn't that patients don't want to pay. It's that the payment process hasn't caught up with how people actually handle money today.
Groceries get paid with a phone tap. So do restaurant bills. But a medical balance still arrives as a paper statement with instructions to write a check and mail it back.
That friction adds up fast. Based on our internal data, over 40% of patients who receive an SMS payment link pay within 48 hours. Compare that to the typical 45 to 60-day paper statement cycle, and the opportunity becomes very clear.
This is where eClinicalWorks text-to-pay changes the game. Instead of waiting weeks for a check, your billing team can send a secure SMS payment link the same day a visit is adjudicated.
The patient gets a text, taps the link, pays in 30 seconds, and the payment hits the eCW billing module automatically.
This article breaks down why the old paper-based model is hurting enterprise RCM, how a text-to-pay workflow solves it, and what real results look like when SMS billing connects to eCW.
Enterprise eCW networks are built on strong technology. Claims get processed. ERAs get posted. Denials get managed.
But that sophistication stops the moment the workflow hits the patient responsibility portion of the bill.
After a visit is adjudicated, the patient balance exits the EHR and enters a much older process. A paper statement gets generated, batched with thousands of others, sent to a print vendor, and mailed. On average, that statement reaches the patient 7 to 14 days after it was created.
Then the patient opens it, maybe. Sets it aside to pay later, probably. Forgets it, often. Thirty days later, a second statement goes out. The billing team eventually escalates to phone calls. Some balances get written off entirely.
The eCW billing module is modern. The collection channel feeding into it is not.
Printing and mailing statements is not just slow. It's expensive. Each paper statement costs between $1.50 and $3.00 when you factor in printing, paper, envelopes, postage, and vendor fees.
A 55-provider eCW network sending 18,000 statements a month spends $27,000 to $54,000 every year on first-round statements alone. Add second and third rounds for unpaid balances, and the cost grows fast.
Add staff time for manual payment posting and phone follow-up, and patient collections become one of the most expensive, labor-heavy parts of the revenue cycle, with the worst return.
Every day a balance goes uncollected, the odds of collecting it drop. Industry data shows that patient balances past 90 days collect at dramatically lower rates than those within 30 days.
Yet the paper statement cycle virtually guarantees most balances won't be touched for 30 to 45 days at a minimum.
By the time a second statement reaches the patient, the visit feels abstract. The motivation to pay fades. The statement-based model doesn't just delay payment. It actively reduces the chance of payment.
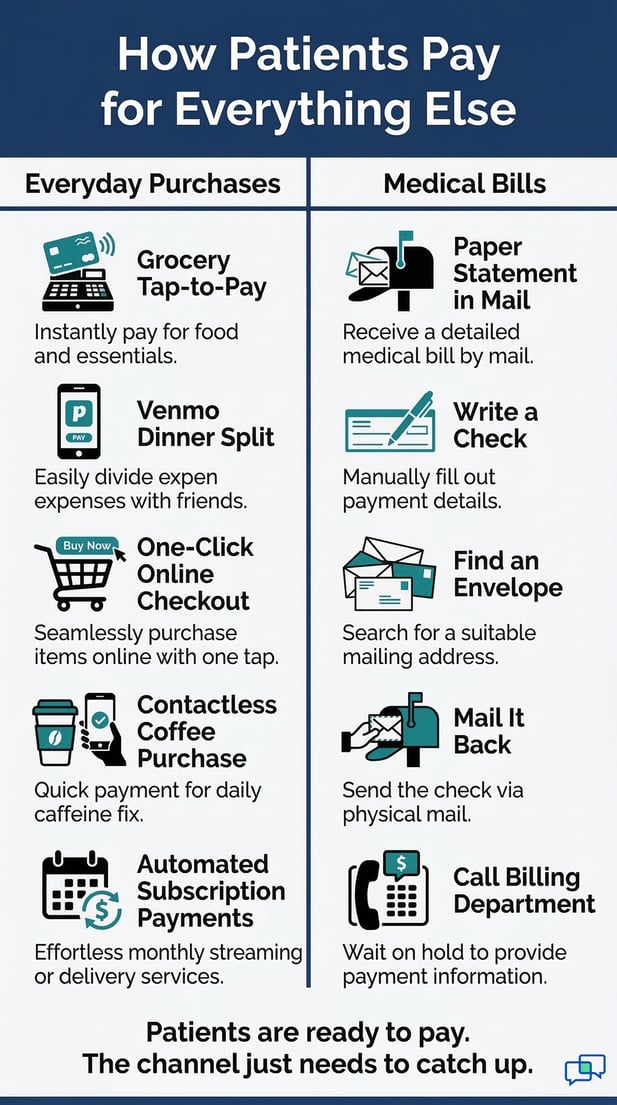
Patients today split a dinner bill in seconds with a mobile app. They check out online with one tap. Then they get a paper bill from their doctor and instructions to find an envelope, write a check, and mail it.
The friction isn't just inconvenient. It's out of step with how payments work in every other part of life. A patient who would pay a $45 copay in 15 seconds via text link will delay or forget that same payment when it arrives as paper two weeks later.
The payment willingness is there. The payment channel just isn't.
|
The statement isn't failing because patients can't pay. It's failing because it asks them to pay in a way nobody does anymore. |
Curogram adds a direct digital payment channel to the eCW billing workflow. The moment visit adjudication sets a patient balance, the system triggers a secure SMS payment link to the patient's phone. No waiting. No printing. No mail.
The payment link opens a mobile-optimized page. It shows the balance amount, provider name, date of service, and payment options: credit or debit card, Apple Pay, Google Pay, and HSA or FSA card. The patient taps, pays, and gets a confirmation text.
The payment then posts to the eCW billing module automatically. It appears exactly as if the patient paid at the front desk, complete with transaction details for audit purposes. Billing staff doesn't need to manually enter anything.
This is what eClinicalWorks accelerate patient collections via mobile payment looks like in practice: the entire cycle, from adjudication to collected payment, happens in hours, not months.
For enterprise networks, Curogram provides a real-time dashboard that tracks payment link delivery, open rates, conversion rates, and total collected. Results can be broken down by provider, location, payer, and balance range.
Billing directors can see which locations are closing balances fastest, which patient groups respond best to SMS payment requests, and where follow-up is still needed. The data is there immediately, not buried in a monthly statement report.
Curogram connects to eCW's billing module through the API, pulling patient responsibility balances after adjudication and posting collected payments back in real time. This integration removes a major source of manual work: payment posting.
For billing teams managing reconciliation across dozens of providers and sites, this saves hours every day and removes posting errors.
The eCW patient payment text link workflow runs automatically, requiring no manual steps between the patient payment and the eCW record.
Text-to-pay works across every specialty in an enterprise eCW network. A cardiology patient pays a specialist copay. An orthopedic patient handles a surgical facility fee.
A primary care patient clears a copay. A dermatology patient pays for a cosmetic procedure out of pocket.
The payment link adapts to the balance and context. For networks with high-deductible health plan patients, which are increasingly common in multi-specialty settings, text-to-pay is especially impactful. The reminder > visit > payment flow creates a seamless experience.
Patient responsibility amounts are larger, and the cost of paper-based friction is higher for both the network and the patient.
Collection Method Comparison
|
Factor |
Paper Statement |
SMS Text-to-Pay |
|
Time to Patient |
7–14 days after generation |
Seconds after adjudication |
|
Average Collection Timeline |
45–60 days |
24–48 hours |
|
Cost Per Transaction |
$1.50–$3.00+ |
Fraction of paper cost |
|
Manual Posting Required |
Yes |
No — posts to eCW automatically |
|
Patient Payment Method |
Check by mail |
Card, Apple Pay, Google Pay, HSA/FSA |
|
Staff Follow-Up Needed |
Frequent |
Minimal |
Switching to an SMS billing enterprise healthcare workflow doesn't just change how payments come in. It reshapes the entire revenue cycle timeline. The shift is measurable, and it shows up fast.
Patient balances that used to sit in the 45 to 60-day A/R aging bucket now close within 24 to 48 hours when patients get instant SMS payment links. That's not a small improvement. It's a complete reframe of what normal looks like.
Based on our internal data, over 40% of patients who receive a text payment link pay within 48 hours.
Average days in A/R for SMS-based balances drop to under a week, compared to more than 50 days for statement-based collection.
Statement volume also starts to fall. As more balances get collected before the statement generation cycle triggers, fewer statements need to go out. The cost savings compound over time.
A 55-provider eCW network in the Southeast activated Curogram's text-to-pay. In the first week, the billing director, Rachel, tracked results for 2,400 patient balances that received SMS payment links.
More than 40% of those patients paid within 48 hours. Average days in A/R for text-to-pay balances dropped to under a week.
Statement volume began falling as balances were collected before the generation cycle triggered.
Rachel calculated the monthly savings: reduced printing, lower postage, less manual posting work, and fewer collection calls.
She then projected the annualized impact across the full network. The CFO approved expanding text-to-pay to all locations immediately.
The billing team's focus shifts when SMS payment links do the heavy lifting. Instead of managing statement runs, processing mailed checks, and making collection calls, the team monitors digital payment analytics and works to improve conversion rates.
That's a better use of billing staff time. And it's a better experience for patients, who can clear a balance in 30 seconds without navigating a phone tree or mailing anything.
The math gets compelling fast at enterprise scale. Reduced statement costs. Lower phone-based billing inquiry volume. Less manual payment posting. Faster cash flow. Fewer write-offs on aging balances.
For networks managing revenue cycles across 20 to 200+ providers and multiple locations, Curogram transforms patient collections from a slow, expensive paper process into a same-day digital workflow. And it does it without adding billing headcount.
Reducing days in A/R for an eCW network means more cash on hand sooner. It means fewer balances aging into the uncollectable range.
It means the revenue cycle works the way modern business processes are supposed to work: fast, digital, and measurable.
|
eClinicalWorks handles what patients owe. Curogram handles collecting it. That's the division of work that makes enterprise RCM actually function at scale. |

Enterprise eCW networks lose time and money collecting patient balances through paper statements and phone calls.
The process was built for a world where patients didn't have smartphones. That world is gone.
The patient balance SMS payment HIPAA-compliant solution that Curogram provides isn't a workaround or an add-on.
It's a full replacement for the paper statement workflow, with direct API integration into eCW's billing module and real-time payment posting.
Balances close faster. Statement costs drop. Staff spend less time on manual posting and phone follow-up. Net collection rates improve because patients pay while the visit is still fresh.
Texts carry a 98% open rate, far higher than email or direct mail. When a payment request lands in that channel, patients actually see it. And when paying takes 30 seconds from a phone, most patients who intend to pay actually do.
The eCW billing module is already doing the hard work of calculating what patients owe. Curogram closes the gap between that calculation and the actual payment.
Curogram's platform is PCI DSS compliant for payment processing and SOC 2 Type II certified for data security. The SMS itself contains only the patient's name, provider, balance amount, and a secure link. No sensitive clinical details are in the text.
The payment page is end-to-end encrypted. Card data is tokenized and never stored. A signed BAA covers all PHI-adjacent data. Enterprise compliance teams can review the full security architecture before activation.
Activate text-to-pay at one location. Send payment links for one week of patient balances. Then compare the collection speed and rate against your paper statement baseline.
Book a demo today and start collecting the same day with a text.
Frequently Asked Questions
Curogram connects to eCW through the API. After visit, adjudication sets a patient balance, Curogram pulls that balance, and triggers a secure SMS payment link.
When the patient pays, the transaction posts directly to the correct patient account and encounter in eCW. No manual entry is needed. The payment appears in eCW exactly as if the patient paid at the front desk.
Patients can reply directly to the payment text with questions. That message routes to the billing team through Curogram's smart routing. The billing team can respond via text, answer the question, and the patient can pay right away once the concern is resolved.
This turns a one-way payment request into a two-way billing conversation, without the patient needing to call, wait on hold, or navigate a phone tree.
Text messages have a 98% open rate. Patients see them within minutes, not days. A payment link that arrives on someone's phone while the visit is still fresh takes 30 seconds to act on. A paper statement that arrives 10 to 14 days later competes with other mail and mental clutter. The channel itself drives a faster response.
The SMS message contains only the patient's name, provider, balance amount, and a secure link. No clinical information or sensitive health data appears in the text.
The payment page behind the link is end-to-end encrypted. Card data is tokenized and never stored. Curogram signs a BAA to cover PHI-adjacent data, and the platform is SOC 2 Type II certified and PCI DSS compliant.
Manual payment posting drops significantly because payments post to eCW automatically. Phone-based billing inquiries decrease because patients can text questions and get fast answers.
Statement management work shrinks as more balances close before the print cycle triggers. The team's time shifts toward monitoring digital payment analytics and optimizing conversion rates, rather than chasing paper.

💡 eClinicalWorks billing teams spend a large part of their time managing paper statements, chasing balances, and posting payments by hand. This...

💡 eClinicalWorks patient mobile payment via text link lets patients pay their medical bills in seconds from their phone. No portal login. No app....

💡 Small practices using Practice Fusion text-to-pay SMS payment links are moving away from paper billing for good. Traditional paper statements...