Curogram vs. Artera: EHR Integration Architecture Compared
💡 When evaluating the Curogram Artera EHR integration architecture, the core difference is how each platform routes patient data to the record....
9 min read
.jpg) Mira Gwehn Revilla
:
April 17, 2026
Mira Gwehn Revilla
:
April 17, 2026

Your EHR is the backbone of your practice. Every patient record, every visit note, and every billing code runs through it. So when you add a patient engagement platform on top, how that platform talks to your EHR matters more than most vendors want to admit.
In 2026, practices face a clear fork in the road. One path leads to a direct API pipeline that reads and writes EHR data in real time. The other leads through layers of AI processing that sit between your data and the final action. Both promise better patient engagement. But they deliver it in very different ways.
This is the core question behind any Curogram Luma Health EHR integration architecture comparison. It's not just about features on a spec sheet. It's about how data moves, who controls it, and what happens when something breaks.
Curogram connects to your EHR through a single, direct line. Data goes in, data comes out. No middle steps. Luma Health takes a different path—one that runs data through its Bedrock layer and then its Spark AI engine before anything reaches your workflow. That adds power, but it also adds parts that can fail or need upkeep.
This article breaks down both models side by side. You'll see how each handles data sync, how long setup takes, and what it means for your staff day to day. The goal is simple: give you the facts so you can pick the model that fits your practice—not the one with the flashiest pitch.
Your EHR is the backbone of your practice. Every patient record, every visit note, and every billing code runs through it. So when you add a patient engagement platform on top, how that platform talks to your EHR matters more than most vendors want to admit.
In 2026, practices face a clear fork in the road. One path leads to a direct API pipeline that reads and writes EHR data in real time. The other leads through layers of AI processing that sit between your data and the final action. Both promise better patient engagement. But they deliver it in very different ways.
This is the core question behind any Curogram Luma Health EHR integration architecture comparison. It's not just about features on a spec sheet. It's about how data moves, who controls it, and what happens when something breaks.
Curogram connects to your EHR through a single, direct line. Data goes in, data comes out. No middle steps. Luma Health takes a different path—one that runs data through its Bedrock layer and then its Spark AI engine before anything reaches your workflow. That adds power, but it also adds parts that can fail or need upkeep.
This article breaks down both models side by side. You'll see how each handles data sync, how long setup takes, and what it means for your staff day to day. The goal is simple: give you the facts so you can pick the model that fits your practice—not the one with the flashiest pitch.
When we talk about how a patient engagement platform connects to your EHR, we're really talking about two schools of thought. One keeps things simple and direct. The other adds smart layers that try to do more—but ask more from you in return.
Curogram's model is built on one idea: the same input should always give you the same output. This is what "deterministic" means in plain terms. If a patient texts "yes" to confirm a visit, that status updates in your EHR right away. There's no guesswork. There's no AI trying to figure out what the patient meant.
The data flows both ways through a direct API link. Your EHR sends data to Curogram, and Curogram writes data back to your EHR. This patient engagement platform bi-directional sync means your front desk never has to enter the same info twice. If a patient fills out a form or confirms an appointment through text, it shows up in the chart on its own.
This matters because every extra step is a chance for something to go wrong. With deterministic EHR data write-back, you can trace every action from start to finish. You always know what happened, when it happened, and why. For practices that need to stay on top of records for audits or compliance, that kind of clarity is a big deal.
Luma Health EHR API integration follows a different path. First, your EHR data goes into what Luma calls its "Bedrock" data layer.
From there, it passes through Luma Health Spark AI orchestration—an engine that reads the data and decides how to route it. Only then does it reach the workflow that touches the patient.
This setup can handle complex, multi-step patient journeys. For example, it could trigger a sequence where a patient gets a reminder, then a follow-up survey, then a recall message—all based on AI-driven logic.
But there's a trade-off. More layers mean more places where settings need to be right. Verified users on review sites have noted that the Luma Health configuration complexity can be hard to manage without a tech team.
If the AI engine reads a data point in an unexpected way, the output might not match what you expected. That's the core difference: a rules-based system gives you the same result every time, while an AI layer may vary based on how it's set up.
For a large hospital with a full IT team, extra layers might be fine. But most specialty clinics and mid-size groups don't have that kind of support. They need a system where the staff—not the tech team—can make changes and trust the results.
When your front desk manager can adjust a reminder template and know exactly how it will behave, that's a win. When every change needs a ticket to IT, that's a drag on your whole operation. The choice between these two models shapes how much control your team has over daily workflows.

The best platform in the world won't help you if it takes months to get running. Setup speed is one of the most overlooked factors when picking a patient engagement tool. And the gap between these two systems is wide.
Curogram's direct API design is built to go live fast. Because there's no AI layer to configure or data-routing engine to fine-tune, the pipeline is ready to work almost out of the box. Practices often reach full bi-directional sync within days, not weeks.
Just as important, clinic staff can manage the platform on their own. The interface is simple enough that training takes as little as 10 minutes. Adjusting a reminder, editing a form, or changing a workflow rule doesn't require IT help.
The results speak for themselves. Based on our internal data, Atlas Medical Center cut its no-show rate from 14.20% to 4.91% within three months of going live—a result 3X better than the industry average.
Covina Arthritic Clinic scaled to over 1,100 automated appointment confirmations per month. These outcomes didn't need a tech team to unlock. Staff ran them through the platform's interface.
Luma Health's setup reflects the complexity of its architecture. More layers mean more things to get right before you flip the switch. Verified reviews on TrustRadius from real users describe the initial setup as difficult and note a steep learning curve. For practices without a dedicated IT department, this creates a challenge that goes beyond onboarding.
The issue isn't just the first few weeks. Ongoing changes—like tweaking a workflow or adding a new message sequence—may also need someone with technical know-how. This turns every small update into a task that waits in an IT queue instead of getting done on the spot.
Think of it this way: if your office manager wants to add a new recall message for patients who missed a follow-up, a staff-managed system lets them do it in minutes. A system that requires IT involvement could mean a delay of days or even weeks. Over time, those delays add up and slow down the improvements you're trying to make.

Here's a side-by-side look at how the two platforms stack up across the most important factors:
|
Dimension |
Curogram |
Luma Health |
|
API Architecture |
Direct bi-directional EHR-to-platform sync |
Multi-layer: Bedrock → Spark AI → Orchestration |
|
Data Write-Back |
Real-time discrete data sync |
AI-processed, orchestrated write-back |
|
Configuration Model |
Staff-managed, rules-based |
IT-dependent, AI configuration required |
|
Setup Speed |
Days (rapid out-of-the-box deployment) |
Weeks to months (enterprise configuration cycle) |
|
Workflow Results |
Same input always gives same output |
Variable based on AI model behavior and config state |
|
Ongoing Upkeep |
Staff-managed through the platform UI |
IT ticket-driven configuration changes |
A few things stand out in this comparison:
The number of layers in the data path is very different. Curogram's single direct pipeline means fewer points of failure. Luma Health's multi-step pipeline may offer more complex routing, but each step is a spot where errors or delays can creep in.
Look at who manages the system day to day. With Curogram, your staff handles it. With Luma Health, you're more likely to need IT support for ongoing tasks. For a 5-provider specialty clinic, that could mean the difference between solving a problem in five minutes or waiting two days for a support ticket to clear.
Consider the predictability of results. A deterministic system gives your team confidence. When they set up a workflow, it does what they expect, every single time.
A system that relies on AI interpretation may produce slightly different results depending on how it reads the data at any given moment. For clinical workflows where consistency matters—like appointment confirmations or medication reminders—that's not a small detail.
Based on our internal research, Curogram clients see an average appointment confirmation rate above 75%, driven in large part by the reliability of the direct sync model.
Picking a patient engagement platform isn't just a software decision. It's an operational one. The integration model you choose will shape how your team works every day for years to come.
Here are three questions every practice should ask before making a choice:
If you have a full-time IT staff member or a managed services partner, you may be able to handle the demands of a multi-layer system. But if your office manager is also your tech support (which is the reality for most specialty clinics), you need a platform that doesn't require technical skills to manage day to day.
Some processes are fine with a bit of flexibility. But others—like confirming appointments or sending HIPAA-compliant messages—need to work the same way, every single time. If your practice relies on consistent, auditable results, a deterministic model is the safer path.
If you need results fast, a platform that goes live in days gives you a head start. If you have the luxury of a long rollout period and dedicated project managers, a more complex system might not be a problem. But for most growing practices, time-to-value is a real concern.
The honest truth is that AI-driven orchestration is an impressive piece of technology. No one is saying otherwise. But the question you should be asking isn't "Is this technology innovative?" The question is "Does this technology serve my practice's reality?"
For specialty and multi-location practices that value staff control, fast setup, and reliable results, Curogram's direct bi-directional architecture removes the complexity that often comes with platforms built around layered AI engines. It puts your team in the driver's seat instead of making them passengers who depend on IT to change the route.
The way a platform connects to your EHR is not a minor technical detail. It defines how your team works, how fast you can launch, and how much control you keep over your own workflows.
Curogram and Luma Health both aim to improve patient engagement. But they get there through very different paths. Curogram's direct, rules-based API sync gives you real-time data flow with no middle layers. Your staff can manage it. Your results are the same every time. Luma Health's Spark AI orchestration offers more complex routing, but it comes with added layers, longer setup, and a heavier lean on IT resources.
For most specialty and mid-size practices, the math is simple. You need a system that works the day you turn it on. You need your front desk team to handle updates without filing a support ticket. And you need to trust that when you set a workflow, it does exactly what you told it to do.
Based on our internal data, practices using Curogram see no-show rate drops that are 3X better than the industry average. They see confirmation rates above 75%. And they reach those numbers in weeks—not quarters. These aren't results that require a team of engineers to unlock. They come from a platform designed to let clinic staff run the show.
The choice between these two models comes down to what your practice needs right now. If you want simple, fast, and reliable EHR integration that your team controls, Curogram was built for exactly that.
Put your team in control of your workflows. Request a demo to see how your staff can manage everything without IT tickets.
Luma Health's Spark AI engine processes EHR data through multiple layers (Bedrock data ingestion → AI interpretation → orchestration routing) before syncing. Curogram uses a direct bi-directional API that writes data back to the EHR in real-time without intermediate AI processing. This architectural difference means Curogram delivers more predictable, deterministic data sync with lower configuration overhead.
Curogram provides a universal bi-directional integration framework designed to work across nearly any EMR system. While Luma Health also supports broad EHR integration, its orchestration model requires more configuration to customize per-EHR workflows. Curogram's approach focuses on reducing double data entry through direct API sync that clinic staff can manage independently.
Curogram case studies document rapid deployment timelines: Atlas Medical achieved a no-show rate reduction from 14.20% to 4.91% within three months of going live, indicating fast integration and workflow activation. Verified Luma Health reviews on TrustRadius and G2 cite difficult setup processes and high learning curves, suggesting longer time-to-value for comparable functionality.
A deterministic system gives the same result for the same input every time. This means staff can trust that confirmed appointments, form submissions, and reminders behave the same way without surprise variations.
Start by asking: Can your staff manage the platform without IT help? Do you need results in days or can you wait months? If speed and staff control matter most, a direct bi-directional sync model will likely serve you better.
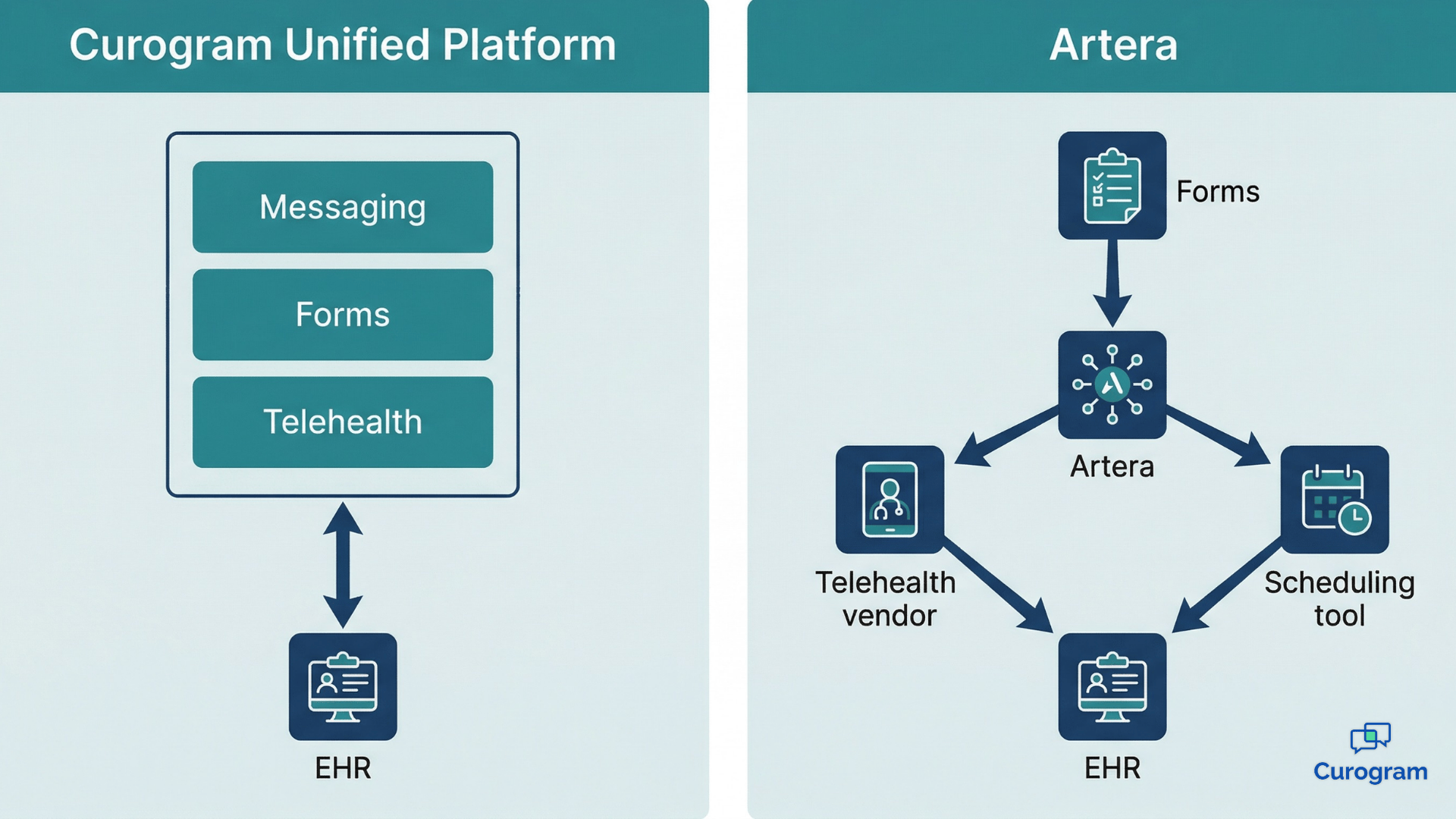
💡 When evaluating the Curogram Artera EHR integration architecture, the core difference is how each platform routes patient data to the record....

💡 The Curogram Phreesia EHR integration architecture debate comes down to one key question: what data reaches your clinicians first? Curogram's...

💡 Curogram and Luma Health both help clinics manage patient engagement, but they take very different paths. The choice in Curogram vs Luma Health...