Curogram vs Artera: Streamlining Clinical Workflows for Practices
💡 The difference between Curogram and Artera is operational. Curogram unifies patient messaging, intake forms, reminders, telehealth, recalls, and...
10 min read
Aubreigh Lee Daculug
:
April 28, 2026
Your practice is losing $25,000 a month to no-shows. You know it. Your office manager knows it.
And yet the solution sitting in your tech stack is a middleware hub that connects to three separate vendors — each with its own contract, renewal cycle, and IT setup — just to send a patient a text message.
It sounds simple. It isn't.
Most medical practices evaluate patient communication platforms the same way: they look at the feature list, check the integration boxes, and compare the monthly subscription price.
Two-way texting? Check. Appointment reminders? Check. EHR integration? Check. Both platforms have it. Done.
But that comparison skips the most important question: what does it actually cost to run this thing — and what is it worth when it works?
Think about this for a moment. Imagine you sign up for a messaging hub. Then you need a separate vendor for digital patient intake forms. Another for telehealth. Another for online reputation management.
And now you need your IT team to maintain all of those connections, debug them when an EHR upgrade breaks the chain, and re-map endpoints every time one vendor updates their API.
That is the hidden architecture behind middleware orchestration. And it has a price tag that never shows up on the original quote.
This article breaks down the real curogram artera cost comparison ROI — not just what you pay for each platform, but what each platform costs you in total, and what each one earns back.
We will quantify the vendor contracts, the IT overhead, and the revenue recovery gap.
By the end, you will have a clear picture of why feature parity does not equal cost parity, and why the platform decision your practice makes today is really a financial operations decision.
The math matters. Let's walk through it.
When health systems sit down to compare patient communication platforms,
The conversation usually starts with features:
Does it do two-way texting? Can it send appointment reminders? Does it connect to our EMR?
Both Curogram and Artera check those boxes. So practices often assume the platforms are economically equivalent and make the decision based on price — or, worse, on which platform they heard about first.
That is a costly mistake.
Feature parity does not equal cost parity. The way a platform delivers those features determines how much it costs to run, how much IT staff time it consumes, how many vendor contracts you need to manage, and ultimately how much revenue it helps you recover.
These are the metrics that determine whether a platform is a smart investment or an expensive liability.
The patient communication platform TCO — the total cost of ownership — is the full picture.
It includes every dollar you spend to make the platform functional: the core subscription, any additional vendor contracts the platform depends on, implementation fees, integration maintenance, and the ongoing cost of IT staff time spent keeping the system stable.
For middleware orchestration platforms, that number is significantly higher than the subscription line suggests.
Artera's model delivers value by centralizing your patient-facing communication thread. That is a real capability. But the economic structure behind that thread is where the complexity — and the cost — lives.
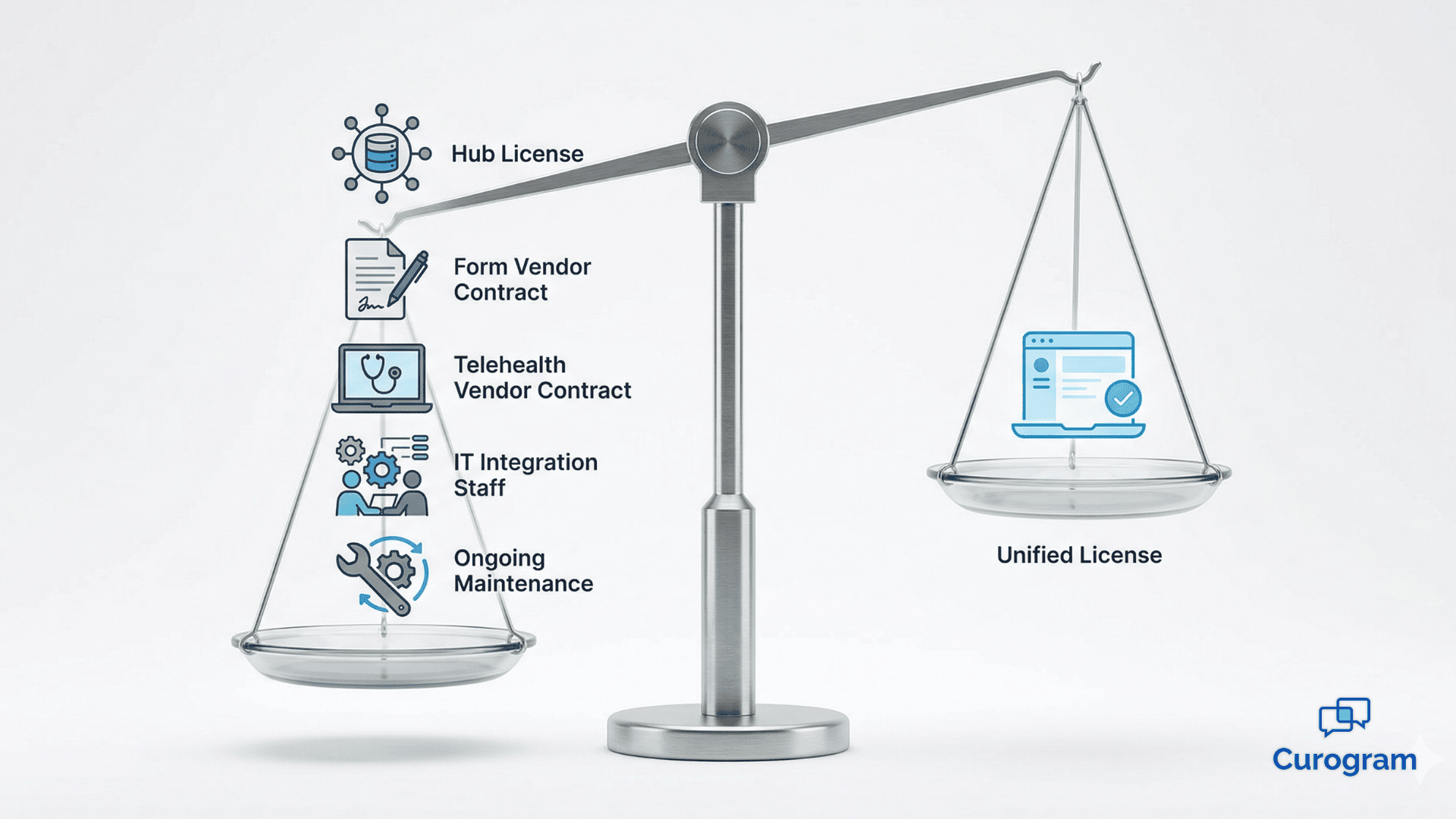
A typical Artera deployment starts with the hub subscription. That covers the messaging orchestration layer. But the hub is not a complete platform. It requires additional vendor contracts to deliver the full feature set that practices actually need.
Here is what that looks like in practice:
Each of those vendor relationships carries its own licensing fee, implementation cost, and annual renewal cycle.
That is three to five separate contracts — each with their own account manager, invoice, and support escalation path — to run a communication stack that most practices think of as one system.
Beyond the subscription costs, middleware orchestration requires middleware orchestration cost in IT labor. Your IT team needs to map endpoints between each vendor and your EHR.
They need to maintain those connections when your EHR upgrades.
They need to troubleshoot write-back failures when data does not flow correctly across the multi-hop chain.
That is not a one-time setup cost. It is an ongoing operational overhead that grows every time you add a vendor or your EHR releases an update.
For practices already spending $800 to $1,000 per month on paper-based billing and losing $20,000 to $30,000 monthly to no-shows, stacked vendor costs are not just inconvenient.
They are a serious drag on a margin that cannot afford it.
Cost reduction is only half of the economic story. The other half — the half that can actually change the financial trajectory of your practice — is revenue recovery.
And this is where the architectural difference between a middleware hub and a unified platform becomes financially significant.
No-show revenue recovery is the most direct measure of a patient communication platform's economic value. Every missed appointment is a provider time slot that cannot be resold, a room that sat empty, and revenue that walked out the door.
The industry average no-show rate for outpatient medical practices is between 10% and 15%.
For a practice seeing 100 patients per day at an average visit value of $200, even a 10% no-show rate represents $20,000 in lost monthly revenue.
Practices with higher no-show rates — or higher average visit values — lose significantly more.
Curogram clients see no-show rates that are 53% lower than the industry average.
Atlas Medical Center reduced their no-show rate from 14.20% to 4.91% in three months — a reduction of more than nine percentage points.
For a practice losing $25,000 per month to no-shows, a 53% reduction recovers $13,250 every month. That is $159,000 per year in revenue that was previously being left on the table.
This is what no-show revenue recovery looks like when the automation runs natively inside the platform rather than through a multi-vendor chain.
Patient recall is the second revenue recovery mechanism that most practices dramatically underestimate. Patients who have cancelled, lapsed, or simply fallen off your schedule represent a recoverable revenue pool — but only if your platform can reach them efficiently.
One multi-location Curogram client ran a native SMS recall campaign and achieved a 35% appointment reconversion rate.
That single campaign recovered 1,240 patients. If the average appointment value for that practice was $150, 1,240 recovered patients represents $186,000 in revenue from one campaign.
Because the recall capability is native to the Curogram platform, there is no additional vendor cost to deploy it.
The same subscription that runs your appointment reminders runs your recall campaigns. In the Artera model, recall typically requires additional configuration or a third-party tool — adding another contract to the stack.

The third economic impact is the one most practices think of last: online reputation.
New patient acquisition through organic search is directly influenced by your Google review volume and rating. Practices with strong review profiles attract more new patients without spending on paid advertising.
A multi-location Curogram client generated 1,064 new five-star Google reviews in three months through Curogram's automated patient survey and review request workflow. Each of those reviews contributes to the practice's search visibility and organic new patient flow.
For a practice where a new patient is worth $500 to $1,500 in lifetime value, reputation-driven patient acquisition is a meaningful and measurable revenue channel.
In a middleware model, reputation management typically requires either a separate vendor or manual staff effort — neither of which is as consistent or scalable as native automation.
The table below maps the full economic comparison between Curogram's unified platform and Artera's orchestration middleware model. This is not a subscription-to-subscription comparison.
It is a total cost of ownership analysis that includes every vendor contract, IT resource cost, and revenue recovery differential that determines the true financial impact of each platform.
| Cost or Revenue Category | Curogram (Unified Platform) | Artera (Orchestration Middleware) |
|---|---|---|
| Core Platform License | Single subscription — all modules included | Hub subscription (messaging orchestration only) |
| Digital Intake Forms | Included — native smart forms | Separate vendor contract required |
| Telehealth | Included — native module | Separate vendor contract required |
| Reputation Management | Included — native Google Reviews integration | Separate vendor or manual process |
| Patient Recall | Included — native SMS recall | Additional configuration or vendor required |
| IT Integration Resources | Lean — one integration path to EHR | Heavy — multi-vendor endpoint mapping and maintenance |
| No-Show Revenue Recovery | 53% lower no-show rates; $10,600–$15,900/month potential recovery | Dependent on multi-vendor chain reliability |
| Patient Recall Revenue | 35% reconversion; 1,240 patients recovered (example campaign) | Dependent on third-party vendor performance |
| Reputation-Driven Acquisition | 1,064 new 5-star reviews in 3 months | Dependent on third-party reputation vendor |
| Total Vendor Contracts | 1 | 3–5+ |
For a practice already running on tight margins, the right column is not just more expensive — it is more fragile. Every vendor in the chain is a potential point of failure, a separate renewal negotiation, and another monthly invoice.
The appointment confirmation rate for Curogram clients exceeds 75%.
That means more than three out of four scheduled patients confirm their appointment before the visit date.
The practical impact: fewer last-minute gaps, less wasted provider time, and fewer follow-up calls for your front desk staff to make.

Here is a cost that almost never appears in a platform comparison: the ongoing IT labor required to keep a multi-vendor integration stack operational.
Every vendor connected to Artera's middleware hub represents a separate integration surface.
When your EHR releases a major update, every vendor endpoint needs to be re-validated.
When one vendor changes their API, the integration breaks until someone on your IT team maps the new connection.
When data does not write back correctly across the multi-hop chain, troubleshooting requires coordinating between multiple support desks — each blaming the other.
This is the healthcare vendor consolidation savings argument at its most concrete. Every vendor you eliminate is one less integration to maintain, one less renewal to negotiate, and one less support escalation to manage.
For IT teams at medium-to-large practices, that is real staff time — measured in hours per month, not minutes.
Curogram's single-platform architecture requires maintaining one integration path to your EHR. One connection. One support relationship. One renewal cycle. When something breaks, you call one team.
For organizations that have calculated their true middleware orchestration cost — including the IT labor component — the vendor consolidation savings alone often justify the platform switch.
Let's build a realistic scenario for a mid-sized primary care practice to make these numbers concrete.
Assume this practice sees 80 patients per day, five days per week, at an average visit value of $180. Their current no-show rate is 12%.
Monthly no-show losses: 80 patients/day × 22 days/month × 12% no-show rate × $180/visit = approximately $38,000/month in lost revenue.
A 53% reduction in no-show rates (Curogram's documented outcome) recovers $20,140 of that every month. That is $241,680 per year — from one feature.
Now add the IT overhead. Assume your IT team spends 10 hours per month maintaining multi-vendor integrations at a fully loaded cost of $75/hour. That is $750/month, or $9,000/year in IT labor for integration maintenance alone.
Add the additional vendor contracts: a digital intake vendor at $300/month, a telehealth vendor at $400/month, and a reputation management tool at $200/month. That is $900/month — $10,800/year — on top of the Artera hub subscription.
The total additional cost of the middleware model: $9,000 (IT) + $10,800 (additional vendors) = $19,800/year before accounting for the revenue recovery differential.
The revenue recovery differential — $241,680/year in recovered no-show revenue — is the number that reframes the entire decision. The platform that costs slightly more per month on the subscription line may be recovering ten times that in clinical revenue.
That is not a technology decision. That is a financial operations decision.
There is a number your practice manager already knows. It might be $15,000 a month. It might be $30,000. It is the revenue that walks out the door every month in the form of no-shows, lapsed patients, and new patients who found a competitor with better Google reviews.
The question is not whether your current communication platform has the right features. The question is whether it is actually recovering that revenue — or whether it is adding cost while leaving the problem unsolved.
Practices that have made the curogram artera cost comparison ROI calculation honestly — accounting for every vendor contract, every IT maintenance hour, and every dollar of recoverable no-show revenue — consistently find that the multi-vendor middleware model costs more and earns back less.
Not because Artera lacks capability, but because the architecture of middleware orchestration adds complexity at every layer: more vendors, more integrations, more failure points, more staff time.
Curogram's unified platform eliminates that complexity. One subscription. One integration. One support team.
And native automation that has driven a 53% reduction in no-show rates, 35% patient recall reconversion, and more than 1,000 new five-star reviews for clients in a single quarter.
If your practice is absorbing five-figure monthly losses to no-shows, paying for multiple vendor contracts to run a communication stack, or spending IT hours maintaining a multi-vendor integration chain — those are not fixed costs.
They are recoverable dollars waiting for the right platform.
Schedule a demo with Curogram today and see exactly what your practice's recovery potential looks like. Bring your current vendor stack, your no-show rate, and your monthly patient volume. We will show you the math.
Direct subscription pricing is not compared here, as pricing varies by contract size and configuration. However, the structural economic difference is significant. Curogram's unified platform includes messaging, intake forms, telehealth, reputation management, and patient recall in a single subscription. Artera's orchestration model requires separate vendor contracts for each of those capabilities beyond the core messaging hub. When you add all vendor subscriptions plus IT integration maintenance costs, the aggregate total cost of ownership for the middleware model is substantially higher than the hub subscription price suggests.
Practices with high no-show rates typically lose between $20,000 and $30,000 per month in recoverable revenue. Curogram's documented 53% reduction in no-show rates relative to industry averages translates to an estimated $10,600 to $15,900 in recovered monthly revenue per affected practice. Atlas Medical Center's specific outcome — reducing no-shows from 14.20% to 4.91% in three months — provides a concrete real-world benchmark. For practices with higher patient volumes or higher average visit values, the recovery potential is proportionally greater.
Based on patterns in enterprise healthcare technology deployments, middleware orchestration platforms require ongoing IT resources to maintain multi-vendor endpoint mapping, troubleshoot failures across the data chain, and reconfigure integrations during EHR upgrades. Each connected third-party vendor represents an additional integration surface that needs to be maintained. Curogram's single-platform architecture requires maintaining one integration path to the EHR, significantly reducing ongoing IT resource allocation. For organizations tracking IT staff time as a budget line, this difference is measurable and meaningful.
Vendor consolidation savings refers to the cost reduction that comes from replacing three to five separate vendor contracts with a single platform subscription. In practical terms, it means fewer renewal negotiations, fewer invoices, fewer support escalations, and less IT staff time spent on integration maintenance. For practices currently running a messaging hub plus separate vendors for forms, telehealth, and reputation management, consolidating onto a unified platform can eliminate thousands of dollars in annual licensing fees while also reducing the operational overhead of managing multiple vendor relationships.
Patient recall is a direct revenue recovery mechanism. When a patient cancels or lapses, the ability to reach them via SMS and reconvert that appointment represents recoverable revenue at minimal incremental cost — as long as the recall capability is native to your platform. In a middleware model, recall typically requires additional configuration or a third-party vendor, adding cost and reducing the speed with which you can deploy campaigns. Curogram's documented 35% reconversion rate across a campaign that recovered 1,240 patients demonstrates the revenue potential of native, automated recall running at scale.

💡 The difference between Curogram and Artera is operational. Curogram unifies patient messaging, intake forms, reminders, telehealth, recalls, and...

💡 When comparing patient communication tools, the subscription fee rarely captures the full cost. For practices outside the ModMed ecosystem,...
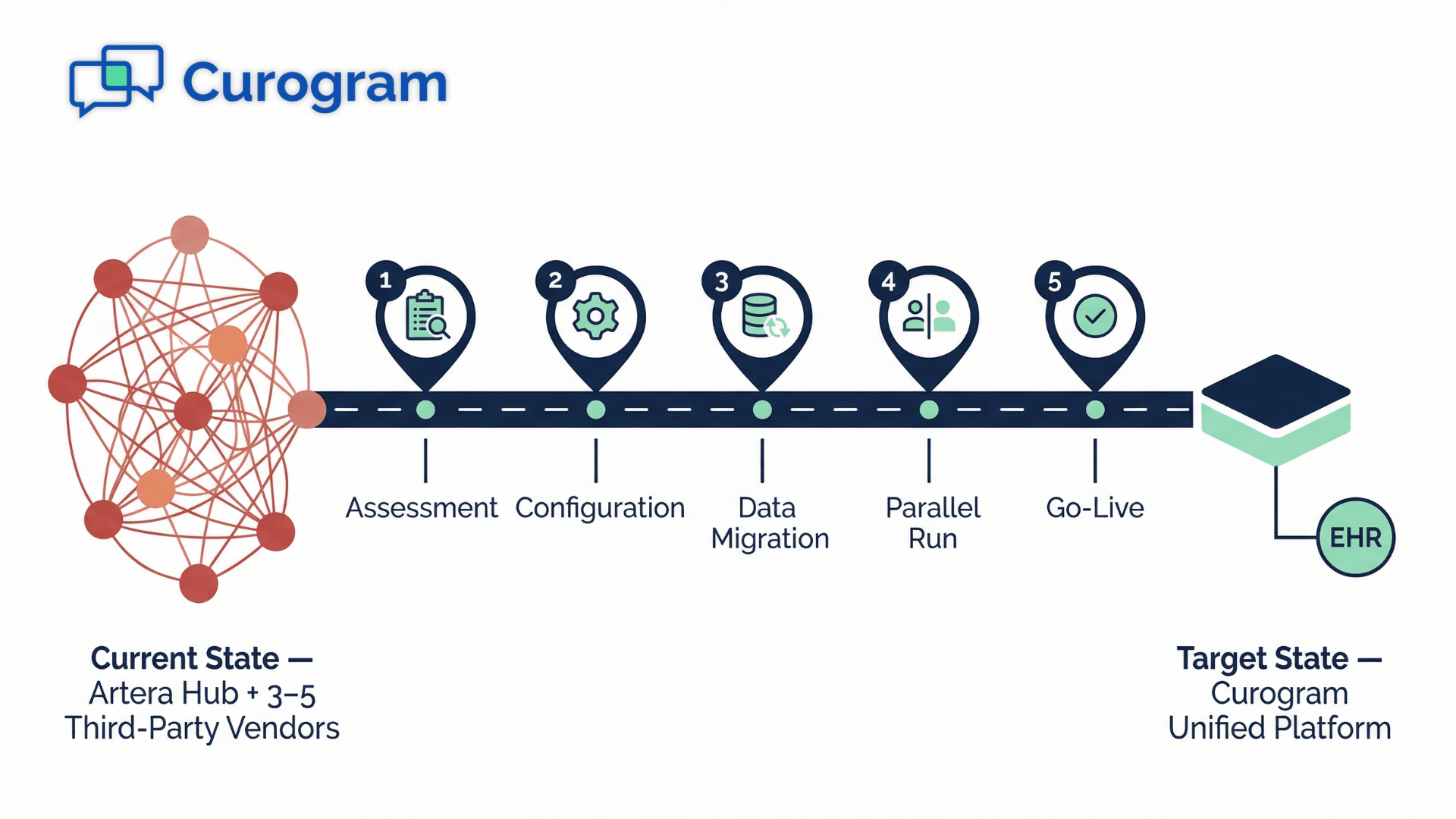
💡 Switching from Artera to Curogram is a vendor consolidation event, not a simple product swap. Artera operates as a middleware orchestration hub,...