RamSoft Telemedicine: Video Consultations Via Text Link
💡 RamSoft imaging center telemedicine video consultation text link HIPAA solutions close the communication gap that drives patient anxiety, day-of...
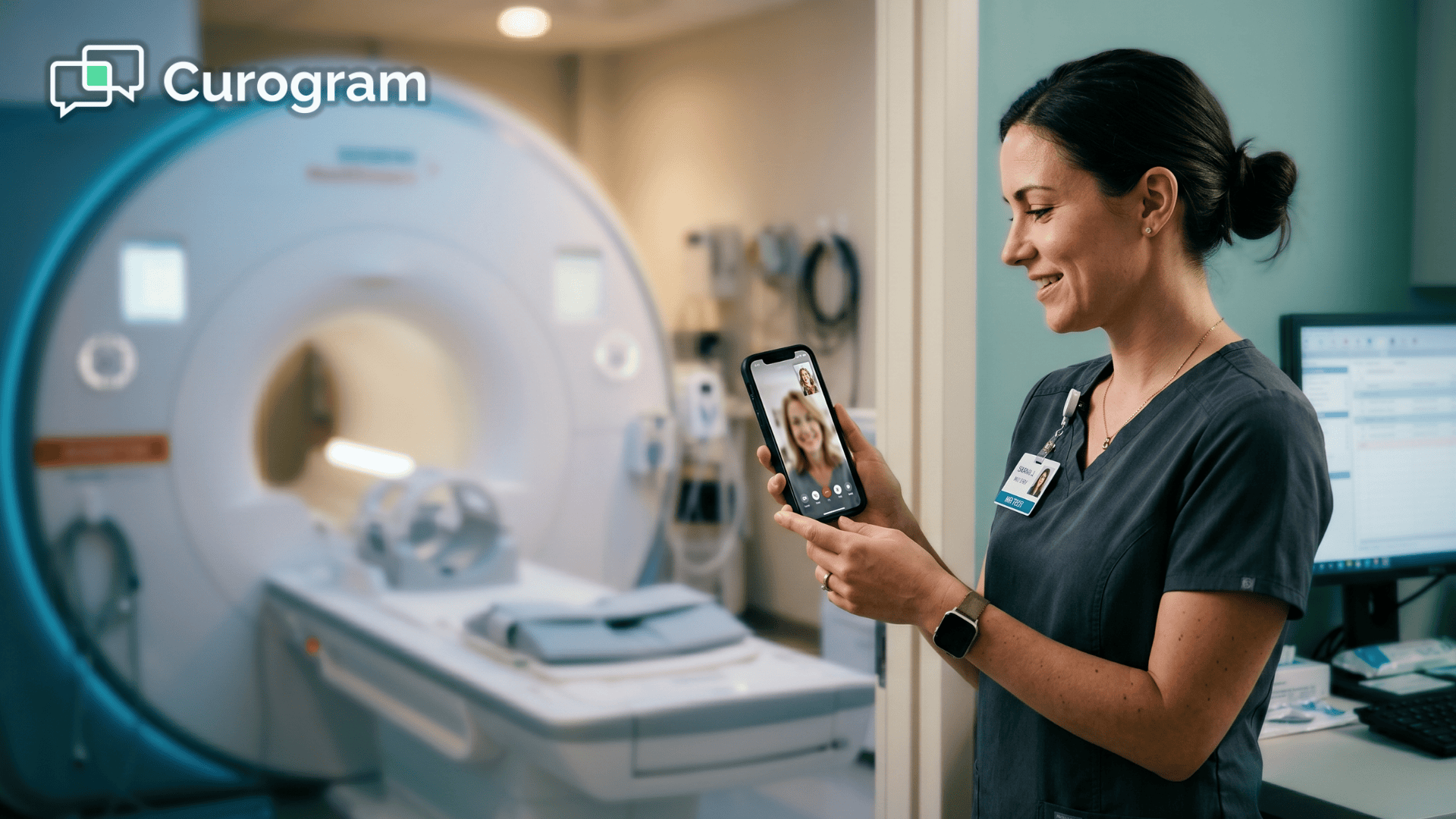
Table of Contents
Your 2:30 PM MRI slot is empty.
Not because the patient forgot. Not because something came up.
They drove to your imaging center, checked in at the front desk, sat in the waiting room, and then — after ten minutes of watching that machine through the glass — walked back to the desk and said, "I can't do this." And left.
You lost the revenue. Your technologist stood idle.
The radiologist's reading queue stalled. And the patient went home without the imaging their physician ordered — a clinical delay that could matter more than any of you know.
This happens more often than most imaging centers are willing to admit. MRI claustrophobia anxiety is not rare. Studies show that between 4% and 20% of patients experience significant anxiety before or during an MRI scan, with first-time patients at the highest risk.
For an imaging center running 30 to 40 studies a day, even a 5% cancellation rate from anxiety alone means losing 1–2 slots daily.
At an average reimbursement of $500–$900 per brain or spine MRI, that's $10,000–$18,000 in lost revenue every month from a problem that is almost entirely preventable.
Here is what makes this harder: the patient wanted to ask questions.
Before their appointment, they googled "MRI claustrophobia" and found Reddit threads, YouTube videos of people panicking inside the scanner, and forum posts about contrast dye reactions. They called your front desk hoping to talk to a technologist.
The receptionist said, "It'll be fine." The patient hung up more anxious than when they called.
There was no one clinical to speak to. No path forward. Just three days of worry building up to a Tuesday they never made it through.
The solution is not complicated. It is a five-minute conversation. But the way that conversation gets delivered — and when — changes everything about the radiology patient experience your center provides.
An MRI anxiety pre-procedure video consultation, delivered 24–48 hours before the study, is the single most effective intervention between referral and scan day that most imaging centers still are not using.
This article explains how it works, why it matters, and what it can do for your center's operations, revenue, and patient retention.
Think about what your first-time MRI patient goes through after they leave their doctor's office with a referral slip.
They schedule with your center. They get a confirmation text or email.
Then they go home and wait — with nothing but their own imagination and Google to fill the gap. That gap is where anxiety grows.
They search "MRI machine" and see images of a narrow, tunnel-shaped bore. They search "MRI claustrophobia" and land on forums where people describe gripping panic, requests to be pulled out mid-scan, and sedation just to get through it.
They read about contrast dye allergies. They wonder if the noise will hurt their ears. They try to picture themselves lying still for 45 minutes inside something that looks like a coffin.
Then they call you.
Your receptionist — who is managing check-ins, phone queues, insurance verifications, and prior authorization paperwork — answers and says, "Don't worry, it's very routine." That is not reassuring. It is dismissive. The patient knows the receptionist cannot actually answer their clinical questions, because the receptionist is not clinical.
This is the gap no one is closing. And it costs your center more than you think.
When a patient cancels day-of from anxiety or abandons the study mid-scan, the damage extends well beyond one lost appointment:
| Impact | Consequence |
|---|---|
| Day-of cancellation | Lost revenue, idle technologist time |
| Mid-scan abandonment | Study failure, possible repeat scan costs |
| Motion artifacts from anxiety | Image degradation, radiologist rereads |
| Negative experience | Patient skips 6-month follow-up |
| No follow-up scan | Delayed clinical findings, lost imaging revenue |
A single anxious patient who leaves without completing their study does not just cost you one appointment.
They cost you the follow-up, the referral relationship, and sometimes the reputation — because a patient who had a bad experience is far less likely to leave the five-star review that brings in new patients.
This means the gap between referral and scan day is not an administrative problem. It is a clinical and financial one.
RamSoft's Blume platform offers something genuinely powerful:
ChatGPT-powered report explanations that help patients understand their imaging results after the study. That is a meaningful leap forward for post-study communication in radiology.
But it does not solve the before.
The patient arriving for their first MRI does not have a report yet.
They do not need help understanding findings. They need someone to explain what the machine will sound like, what the table will feel like, whether they will be able to breathe, and what happens if they cannot handle it.
Those are not questions Blume can answer before the study — because that conversation has to happen with a human.
Your front desk team is excellent at what they do. Scheduling, insurance, check-in, paperwork — these are their lanes.
But clinical preparation for an MRI study is not. When a first-time patient asks whether the contrast injection will hurt, or how they should handle their claustrophobia during the scan, your receptionist does not have the training or authority to answer accurately. And they know it.
So they default to stock reassurances that close the conversation without actually resolving anything:
It sounds helpful. It isn't.
That kind of response leaves the patient with the same unresolved fears they called with — sometimes worse, because now they also feel like no one took their concern seriously enough to actually answer it.
Your MRI technologists are the right people to have this conversation.
They know the machine. They know what patients experience. They can answer questions accurately, describe what the procedure actually feels like, and provide real reassurance based on clinical experience.
But during business hours, they are in the scanner room. They are not available for inbound patient calls.
And there has never been a structured, scheduled way to connect a pre-procedure patient with the technologist who will be running their study.
Until now.
Here is what an MRI anxiety pre-procedure video consultation looks like in practice.
Twenty-four to 48 hours before a patient's scheduled study, they receive a text message from your imaging center.
It reads something like:
"Hi [Name], your MRI is scheduled for Tuesday at 2:30 PM. Would you like a quick video call with your technologist to see the room and ask questions? Tap here."
The patient taps the link. A video call opens instantly in their phone's browser.
No app download. No portal account. No login screen. No friction.
A technologist joins the call. The conversation lasts about five minutes.

That conversation is not scripted or rushed. But it covers a lot of ground:
By the end of that call, the patient has seen the room.
They have heard a calm, clinical voice explain exactly what to expect. They have a face to recognize when they walk through the door on Tuesday.
That is not a minor comfort. That is a complete reframe of the experience before it starts.
This pre-procedure patient consultation is not one-size-fits-all.
Curogram's workflow accommodates different patient needs directly, with each type of concern getting a conversation tailored to it:
Every patient type gets preparation that matches their actual concern. That specificity is what makes first-time MRI fear manageable before it becomes a day-of cancellation.
The operational impact of a structured MRI pre-procedure video call is measurable — and it shows up in multiple places across your center's performance.
Industry research on pre-procedure interventions consistently shows that patients who have a clinical conversation before their study are 30–40% less likely to cancel day-of.
For a center running 25 MRI studies per day, eliminating even 2 anxiety-driven cancellations per week frees up 8–10 slots per month.
At an average reimbursement of $700 per study, that is $5,600–$7,000 in recovered monthly revenue from one workflow change.
Day-of cancellation rate |
| Without pre-procedure call: ~8–12% → With pre-procedure call: ~4–6% |
Calmer patients lie still. That sounds obvious, but the clinical consequences of motion artifacts are significant. Motion-corrupted images require radiologist rereads, possible repeat sequences, or full study cancellation. Each repeat scan costs time, resources, and technologist capacity.
When pre-procedure preparation reduces patient anxiety, motion artifact rates drop — which means cleaner images, faster reads, and fewer costly do-overs.
Motion artifact rate |
| Without pre-procedure call: Elevated → With pre-procedure call: Reduced |
This is the metric most imaging centers overlook. Patients who have a positive radiology patient experience on their first visit are significantly more likely to return for recommended follow-up imaging.
Research on patient satisfaction in imaging settings suggests that patients who feel prepared and well-communicated with are up to 60% more likely to complete a recommended 6-month follow-up study.
That follow-up study is full revenue.
It requires no new referral. It is a direct return on the five minutes you spent preparing the patient before their first scan.
Follow-up compliance (6-month) |
| Without pre-procedure call: ~40–50% → With pre-procedure call: ~65–75% |
In practice, the five minutes a technologist spends on Sunday afternoon could directly influence patient outcomes, imaging revenue, and online reputation — all at once.
One of the most common concerns imaging center directors raise about adding new patient communication steps is this:
"We're already stretched. Where does this fit?"
The answer is that it does not require building something new. It slots into what you already have.
Curogram's platform is the same one sending your appointment reminders and pre-visit intake forms.
The pre-procedure video consultation link goes out through the same communication channel — a text message from the same number the patient already recognizes. To the patient, it is not a new system. It is the next message from your center, arriving at a natural moment in their preparation timeline.

For your staff, the process is straightforward from start to finish:
There is no separate app, no third-party scheduling tool, and no manual coordination required.
The intake forms do the prep work, so the conversation is immediately relevant to that specific patient's situation — not a generic walkthrough.
RamSoft’s workflow already manages the imaging study lifecycle from scheduling through reporting. With RamSoft integration, Curogram connects directly to that timeline at the communication layer.
This means the pre-procedure video call fits naturally into the existing patient communication sequence — after the appointment reminder, before the day-of check-in — without disrupting clinical or administrative workflows.
Blume explains the report after the study. Curogram prepares the patient before it.
Those two tools address different moments in the patient journey, and together they create a more complete imaging center communication model than either delivers alone.
Centers that add pre-procedure preparation consistently report patient satisfaction scores that move from average to significantly higher — not because the imaging changed, but because the communication did.
Here is what Tuesday looks like when the pre-procedure process works.
Your patient receives the video call link Monday morning. They spend five minutes with the technologist, see the scanning room, hear what the machine sounds like, and ask their three questions about contrast.
They go to bed Monday night without dread.
Tuesday at 2:30, they walk in and recognize the technologist from the video call. They feel like they already know this person, this room. The study runs smoothly.
The patient lies still. The images are clean. The radiologist reads without complications.
Before the patient leaves, they mention to your front desk that they were nervous going in but that the call on Monday made all the difference.
Two days later, they leave a five-star review that says:
"I was terrified of MRIs. The technologist called me before my appointment and showed me the room. I actually felt prepared. Best healthcare experience I've had."
That review influences the next anxious first-time patient who is googling your center. That patient books instead of calling around. The cycle continues.
Preparedness is not just a clinical benefit. It is a marketing one. And the evidence shows up in the reviews — five-star mentions of feeling prepared go from rare exceptions to a pattern you can count on.
Pre-procedure video consultations are not a luxury add-on. They are a gap-filler for a problem that imaging centers have been managing with improvised workarounds — reassuring receptionists, generic prep instructions, and hope — for years.
The conversation between referral and scan day is one of the most underinvested touchpoints in the entire radiology patient experience.
And closing that gap does not require more staff, more budget, or more complexity. It requires a structured, scheduled, 5-minute video call that puts a clinical face on the process before anxiety has time to take hold.
Imaging centers that invest in this kind of pre-procedure patient communication see the returns across multiple metrics: fewer cancellations, fewer corrupted scans, higher follow-up compliance, better online ratings, and stronger patient retention.
The outcomes are measurable. The workflow is simple. The barrier to starting is low.
Your 2:30 PM slot should never sit empty because a patient was too anxious to go through with it.
A five-minute conversation on Monday can change that — for that patient, for that slot, and for every referral that comes through your door without knowing what to expect.
Schedule a demo with Curogram to see how MRI pre-procedure video consultations integrate into your RamSoft workflow. See the platform, ask the questions, and find out how quickly your team can begin closing the gap between referral and scan day.
Yes. All Curogram video communications are HIPAA-compliant and fully encrypted end-to-end. Video calls are not recorded by default — they are live conversations only. The patient initiates the call through a unique, single-use text link. The technologist joins from within the HIPAA-secure video interface inside the Curogram platform. No recording or transcript is stored unless the facility explicitly enables optional note-taking. Patient privacy is protected at every step of the process, from link generation through call completion.
Curogram supports a phone call fallback for patients who do not have a smartphone or prefer voice-only communication. If the patient does not tap the video link, the technologist can initiate a standard phone call at the scheduled pre-procedure time. The conversation covers the same preparation content — what to expect, questions answered, reassurance provided — just without the visual element. For elderly patients, non-English speakers, or patients with accessibility needs, a family member or medical interpreter can join the video or phone call to ensure full understanding and appropriate support.
Yes, there are clear clinical boundaries — and they exist to protect both the patient and your staff. The technologist can explain how the MRI machine works, what the patient will experience during the study, how long the scan takes, whether contrast will be used, and how the patient should position themselves. They can also answer logistical questions about what to wear, what to bring, and where to arrive. What the technologist cannot do is diagnose a condition, interpret prior imaging, or discuss any clinical findings — those conversations belong to the radiologist after the study. The pre-procedure call is specifically about preparation and confidence, not clinical assessment.
Less than you might expect. A pre-procedure video call runs about five minutes per patient, and not every patient on your schedule will need one — it is typically offered to first-time MRI patients, patients who flag anxiety during intake, or those with specific clinical considerations like claustrophobia or contrast history. For most imaging centers, that translates to two to four calls per day, most of which can be scheduled during natural gaps between studies — shift start, lunch, or the window between afternoon slots. It is not a new workload. It is a smarter use of time that already exists.
The workflow is not limited to MRI. Any imaging study that tends to generate patient anxiety or requires specific preparation can benefit from a pre-procedure conversation. CT scans with contrast, nuclear medicine studies, and certain interventional radiology procedures are common candidates. The format is the same — a brief, text-linked video call 24–48 hours before the study — and the Curogram platform handles it identically regardless of modality. If your center runs multiple imaging types and sees anxiety-driven cancellations across any of them, the same workflow applies.
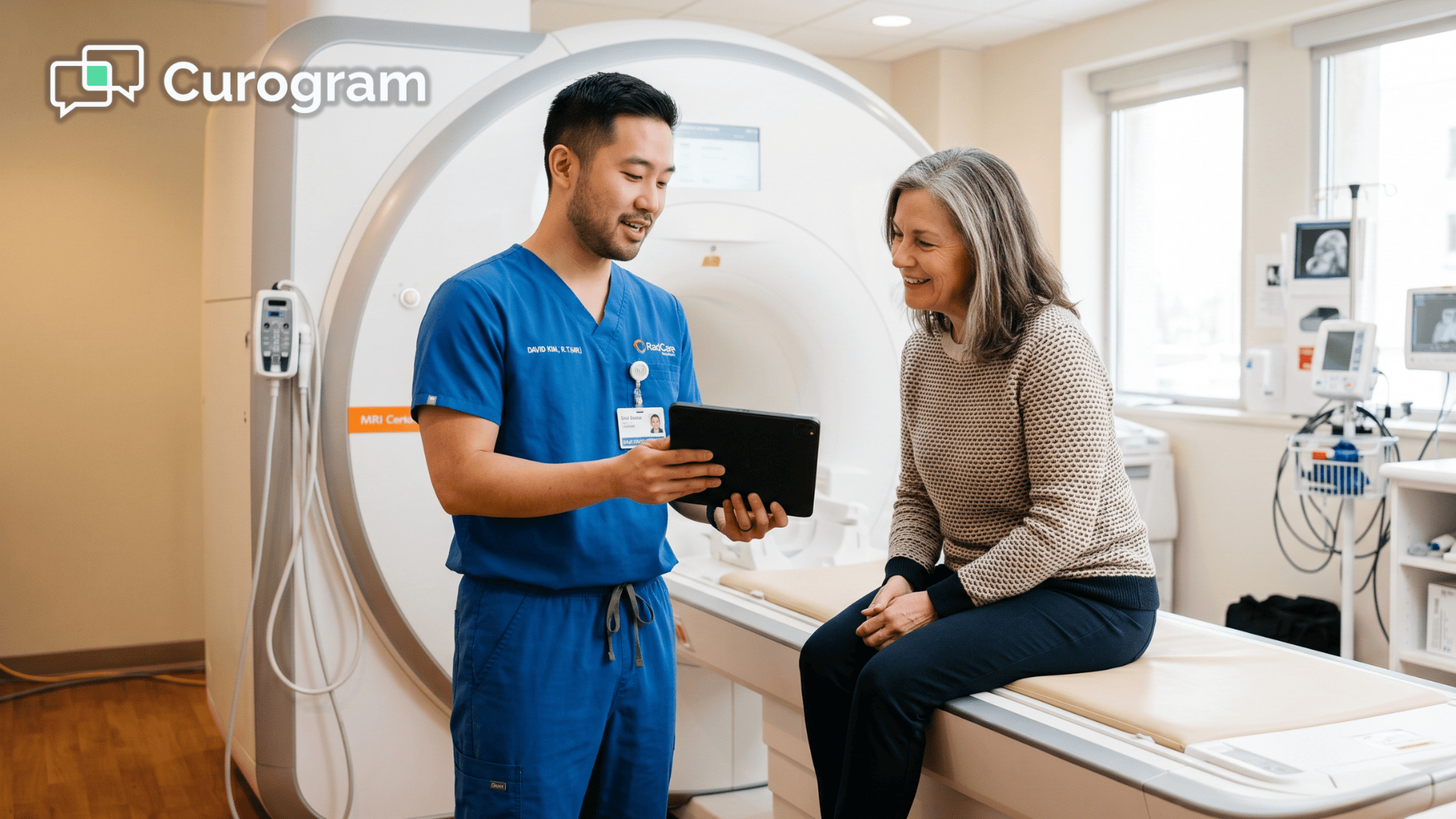
💡 RamSoft imaging center telemedicine video consultation text link HIPAA solutions close the communication gap that drives patient anxiety, day-of...

💡 Imaging center staff lose hours every week to pre-procedure phone calls, delayed physician check-ins, and last-minute cancellations.Curogram,...
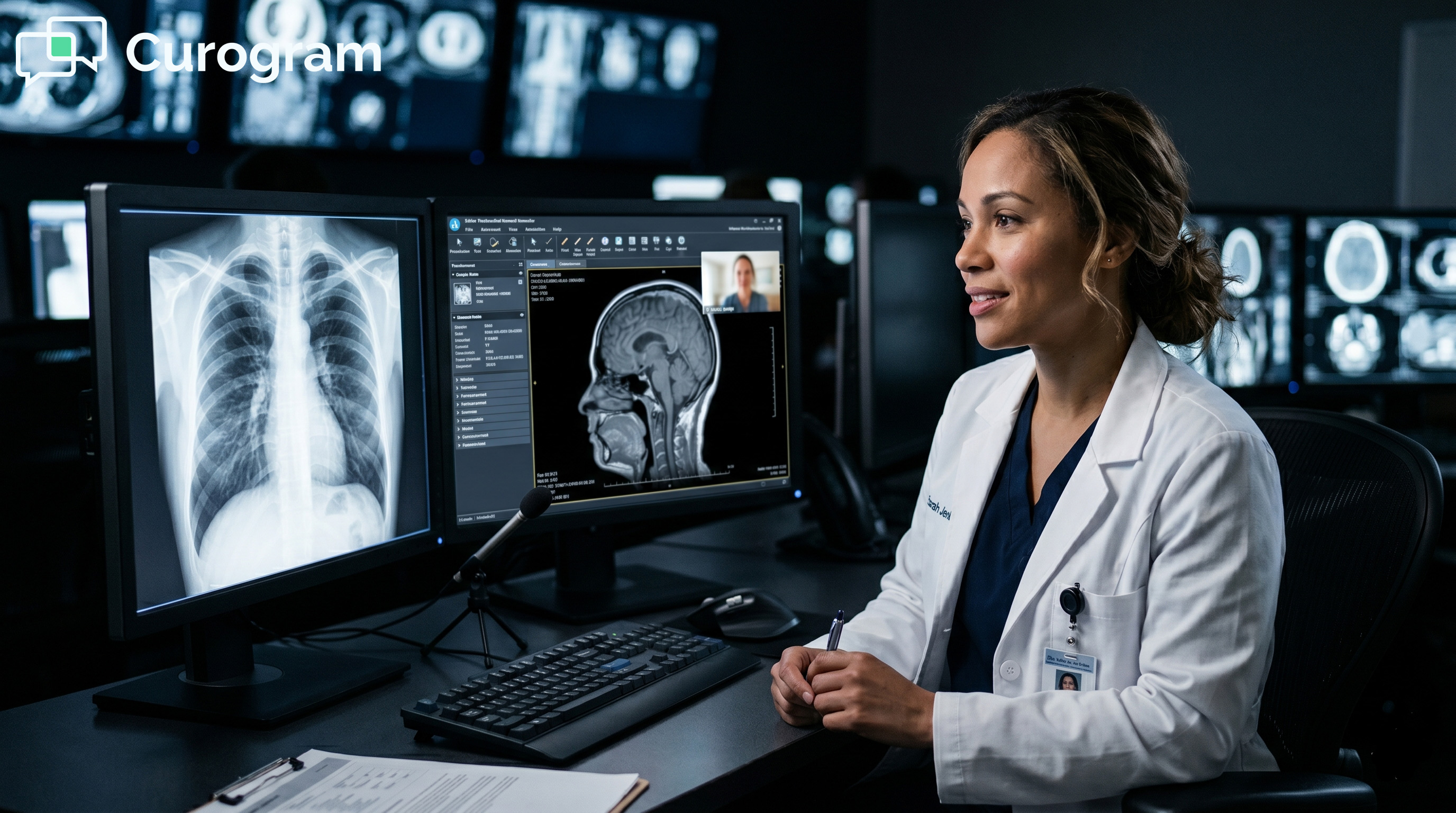
💡 Exa PACS RIS is a leading imaging platform for storing and reading diagnostic images. But it has no built-in way to talk to patients. That gap...