Reputation Management in InSync EMR with Curogram
💡 Reputation management in InSync helps behavioral health practices manage online presence. With automation, you can collect more positive reviews...
Trigger requests automatically after a visit or group session.
Use InSync review automation so staff do not chase every survey.
Capture therapy patient feedback while the experience is fresh.
Route unhappy responses inside the clinic instead of straight to public sites.
Ask short, simple questions that feel safe to answer.
See patterns that help you improve how care feels.
With Curogram, you make feedback part of the care process, not an extra chore for staff or patients.
You probably remember the sting of a harsh online review. You read the words and think about the day it describes. Maybe the lobby was understaffed or the schedule ran late. You remember the faces and the stress. Then you look at your list of patients who were grateful, kind, and quiet. Their voices are missing from the record.
This is the core problem with reviews in behavioral health. People are much more likely to post when they are upset than when they are content. If you only hear from the angriest voices, the picture of your care is incomplete and often unfair.
We saw in our guide for InSync EMR clinics just how impactful online review management can be. In this blog, we explore why it is so hard to manage reviews by hand, especially in a busy behavioral health program. Learn how to use automated review requests to send simple, timed surveys after visits. Let's also see how automation can route bad feedback back to your team instead of going public. By the end, you'll find clear next steps to apply automation to manage your reputation the right way.
You may notice a pattern when you look at your reviews. Many of them come from people who had a very bad day. They might have waited too long, struggled with billing, or felt misunderstood in a session. Their feelings are real and deserve attention. But they are not the whole story.
Many satisfied patients never post anything at all. Research on consumer behavior shows that people are more likely to leave a review when they feel very negative. In healthcare, this means that a small number of very upset voices can shape how your care looks from the outside. Quiet patients who felt seen and supported walk away, feel grateful, and then move on with their lives. Their stories stay with them instead of reaching you or future patients.
You may have tried to fix this by asking staff to invite reviews. Front desk staff might mention it during checkout. Therapists might bring it up at the end of a visit. Sometimes this works. A motivated patient will go home and search for your name and leave kind words. But that usually happens in small numbers.
Most of the time, staff are too busy to remember these requests for every single patient. Behavioral health schedules are full. Crises come up without warning. People need extra time and care. In these moments, asking for feedback feels like the last thing on the list. Manual processes rarely survive the daily pressure of real work. The result is an outreach effort that is inconsistent, staff dependent, and fragile.
When you only hear from unhappy patients, it is hard to know how care feels for everyone else. You may sense that most sessions go well, but you see only a handful of harsh public comments. It feels unbalanced. You may even question your own work or your team’s commitment, even though you know how much effort you give every day.
This missing information also limits your ability to improve. Patient experience studies like CAHPS and HCAHPS show how structured feedback can highlight patterns in communication, environment, and trust. If behavioral health programs only collect feedback from crisis moments, you lose the chance to learn from typical days. Silent satisfied patients remain invisible. Their quiet approval does not guide training, policy changes, or workflow tweaks. You end up steering the ship with only a few loud signals and a lot of guesswork.
Curogram connects to your InSync schedule so that review requests can follow real visits automatically. When a session closes in InSync, that event can trigger a short survey message. You do not have to remember who to ask or when to send the link. Automated review requests InSync workflows turn this into a quiet background process.
You can choose how soon after the visit to send the request. Many programs like to send it within a few hours, while the experience is still fresh. Others prefer a short delay for sensitive therapy sessions. The key is that you decide the rules once, instead of asking staff to make fresh decisions for every patient every day.
Most patients are already comfortable with text messages and email. They use these channels for school, work, and family life. When a review request arrives in the same place as daily messages, it feels normal. You can keep the text short and simple. A few words of thanks, a link, and a clear ask are usually enough.
This is especially important for therapy patient feedback. Many people feel vulnerable after a session. They may not want to open a long form or log into a portal. A brief message that honors their time and emotional energy is more likely to receive a response. InSync review automation gives you the tools to send these requests in a calm, predictable way that fits into real life.
One powerful part of this workflow is internal routing. Not every piece of feedback needs to go straight to a public site. With Curogram, you can design a path where low scores or concerning comments are captured inside the clinic first. This gives you a chance to respond, repair, and learn before that story travels further.
For example, you might send a simple rating question. If a patient chooses a low score, the system can flag that response for a manager or patient experience lead. You can then decide whether to reach out, review the case, or adjust a process. This approach respects the patient’s emotion while also protecting staff from surprise attacks online. It turns negative feedback into a private doorway for improvement instead of a public blow.
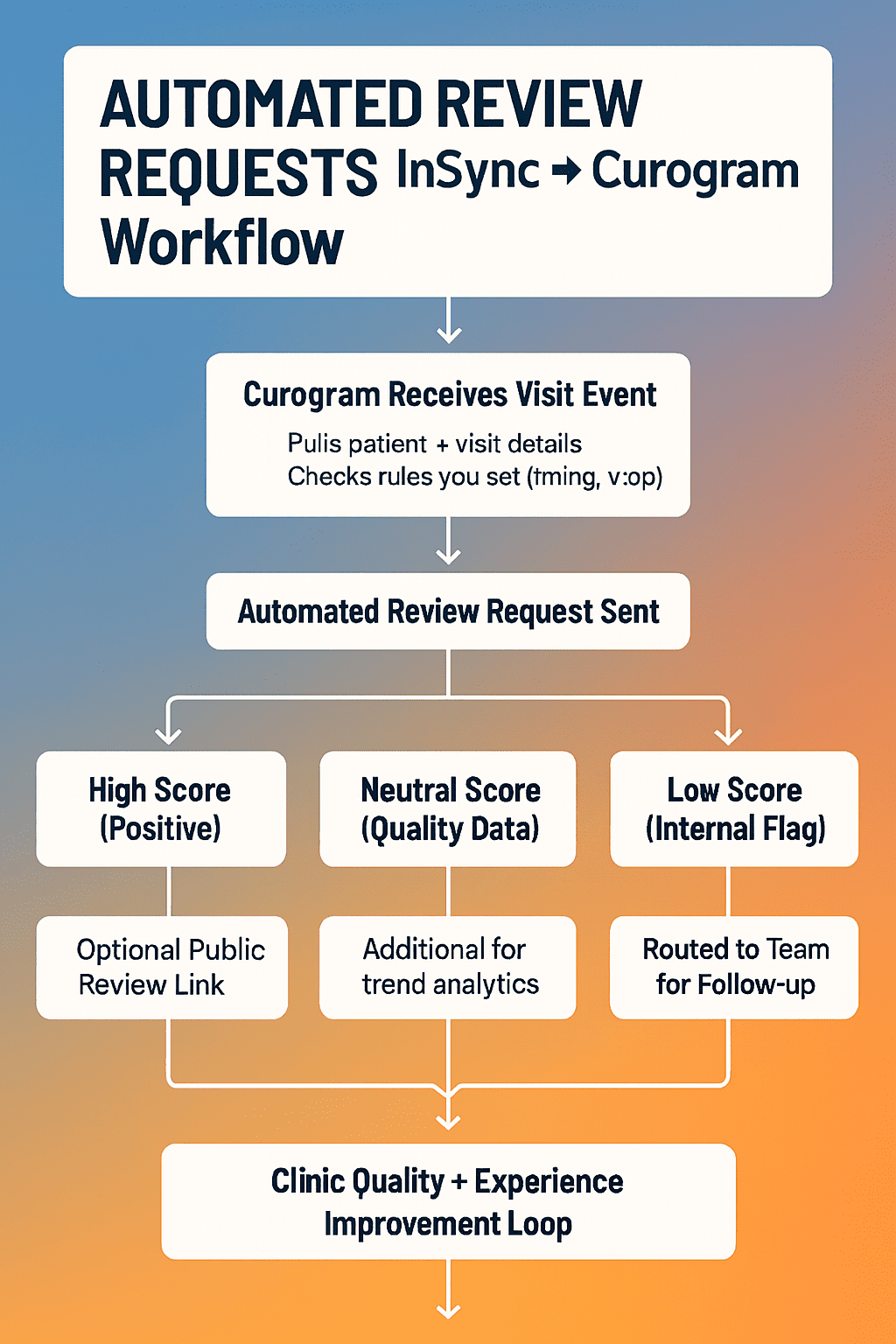
When you move review requests into an automated flow, you remove one more manual burden from your team. Staff no longer have to remember who they asked, who they forgot, or who promised to leave feedback but never did. The system handles those details. Your front desk and clinical staff can use their time for work that truly needs a human presence, such as deescalating a crisis or comforting a worried family.
Over time, this shift changes how the day feels. Instead of feeling guilty for not keeping up with feedback requests, staff know that every patient is invited in the same fair way. That sense of fairness matters. It reduces quiet stress and lets people trust the process instead of trying to manage everything on their own.
From a patient’s point of view, an automated request can feel gentler than a direct verbal ask. When someone is sitting at the front desk after a hard session, they may not want to talk about reviews. They might feel pressured to smile and say yes even when they are exhausted. Later, that request may feel like one more thing they failed to do.
With automated review requests InSync workflows, the invitation comes later, in private. The patient can respond on their own time, in their own space. They can be honest without worrying about hurting someone’s feelings in the moment. In surveys of healthcare consumers, many patients say they want their feedback to shape care, and structured review systems are one way to honor that wish.
Therapy is emotional work. Patients may leave sessions with strong reactions that soften or change over time. If you wait months to ask about their experience, the details blur. Automated requests that follow soon after a visit capture those early impressions. They can reveal how safe patients felt, whether they understood the plan, and what small things made a big difference.
Because therapy patient feedback arrives continuously, you can track patterns. Maybe several patients mention feeling rushed at the end of group. Maybe others mention trouble with the check in process. You can use this information in supervision, staff meetings, or quality projects. It gives you a living picture of how care feels across many days and many rooms.
When you collect feedback only from the most upset patients, your public ratings and internal surveys do not match the real work you see. Automated outreach helps balance that picture. Studies of review behavior show that when more people are invited to share, ratings tend to move closer to the actual average experience.
For a behavioral health program that works hard to deliver kind, consistent care, this balance matters. It does not erase the hard days or the times you fall short. Instead, it lets those moments sit alongside many others where patients felt respected and supported. Staff can read feedback that both challenges and encourages them. That mix is often more motivating than a stream of only negative comments.
Internal routing of low scores does not hide problems. It gives you a safer way to address them. When someone has a bad experience, they often want to be heard more than they want to attack. An internal form can invite them to describe what happened and how it felt. You can respond with empathy and, when appropriate, a clear plan to make things better.
Handling the first wave of anger privately can prevent situations from escalating. It can also reveal deep issues that would never show up in a short public comment. You can identify patterns in staffing, communication, or environment and address them. In this way, negative feedback becomes a source of wisdom instead of only a source of shame.
Behavioral health programs often participate in quality improvement efforts. They track incidents, read chart audits, and review outcome measures. Patient experience data belongs in that same circle. National patient survey programs, such as CAHPS, show that structured feedback can point directly to changes that improve experience and safety.
Automated review workflows give you a steady stream of qualitative data. You can group comments by theme, location, or program. You can look for changes after you adjust a policy or redesign a waiting area. This makes review data feel practical, not abstract. It becomes one more tool you use to protect patients and support staff.
When feedback arrives regularly, you can talk about it in calmer ways. It is no longer a rare crisis when a long, angry review appears online. Instead, staff can treat feedback as a normal part of the work. You can celebrate kind comments together and sit with the painful ones as a team instead of alone.
Team members who rarely hear from patients directly, such as billing or scheduling staff, can also see the impact of their work. They read where patients noticed their patience or clarity. This kind of recognition can fight burnout. At the same time, recurring concerns can spark practical changes in scripts or processes. Conversations start to revolve around “What can we adjust?” instead of “Whose fault is this?”
It is hard not to take a negative review personally, especially in behavioral health, where you pour emotional energy into your work. When you only have a handful of reviews, each one feels huge. A single star rating can sit in your mind for months. That weight can contribute to burnout and doubt.
As your feedback volume grows through automated outreach, each individual comment becomes part of a larger picture. This does not make criticism painless, but it makes it more proportional. You can see that one harsh comment sits next to many that show trust and gratitude. That balance can help staff stay grounded and open to learning.
Picture a behavioral health network with several outpatient sites. Before automation, they had a small number of public reviews, many of them very negative. The average rating hovered around 3.2 stars. Staff felt discouraged because they knew that most patients expressed thanks in person, but those stories never reached the outside world.
The network decided to turn on automated review requests InSync workflows through Curogram. Every completed visit triggered a short survey by text. Low scores went to an internal feedback queue. Higher scores invited patients to share their experience on selected public platforms if they wished. Within six months, hundreds of new reviews appeared, and the average rating rose to around 4.6 stars.
The most important change was not the number. It was the tone of the comments. Many patients wrote about feeling heard, safe, and understood. Staff read these stories and felt their hard work reflected back to them. When negative comments appeared, they often came through the internal route first, which gave the network a chance to call, listen, and repair.
This network learned that automation did not erase hard truths. It revealed them in a more complete way. They discovered repeated concerns about wait times at one site and used that information to adjust staffing. They also noticed praise for particular groups and used that model to strengthen other programs. Feedback became a map instead of a threat.
They also learned that staff buy in mattered. Leaders took time to explain that InSync review automation was not about blaming individuals. It was about seeing patterns and supporting change. As trust grew, staff started to bring feedback into supervision and team huddles. That culture made the technical tools much more effective.
Take an honest look at how you gather and use patient feedback now. Ask yourself how many reviews you receive each month and where they come from. Look at whether the same themes appear again and again. Consider how often you hear from therapy patients in a structured way, not just in passing comments.
When you choose a tool to manage feedback, you are not just choosing software. You are choosing a partner that will touch the most vulnerable moments of your patients’ stories. Curogram is built for healthcare communication, so it treats every message as part of the care experience, not just as data. When Curogram connects to InSync, it uses the schedule you already trust as the starting point for outreach.
When you are ready to explore automated review requests, you do not have to transform everything overnight. Start with one site, one program, or one type of visit. Work with a small group of staff to design message templates that match your values and your patients’ needs. Keep the tone warm, short, and clear.
As responses come in, review them together as a team. Adjust wording, timing, or routing as you learn. Over time, you will build a feedback system that feels like part of your healing work, not a separate technical project.
InSync review automation with Curogram lets you send simple surveys after every visit. You can route negative responses inside the team and listen for patterns across time. It turns reviews into a steady stream of data that supports both care and learning.
Even a small pilot can show you how patients respond when you ask in a kind, consistent way. Over time, you can grow a culture where staff are less afraid of reviews and more curious about what they reveal. In that kind of culture, therapy patient feedback becomes a part of the shared work of healing.
Want to see how easy it is to manage your online reviews? Book a quick demo today.
💡 Reputation management in InSync helps behavioral health practices manage online presence. With automation, you can collect more positive reviews...

💡 Reputation management in DrChrono helps small clinics grow their practice. They can attract new patients effortlessly through the following...

💡 Reputation Management in Dolphin Management empowers orthodontic and oral surgery practices. These clinics can grow through automated, compliant,...