One-Tap Patient Payments for Oracle Health | No Portal | Curogram
💡 SMS payment collection revenue cycle ROI healthcare improves three numbers fast: payment conversion, days-in-A/R, and bad debt. Paper statements...
10 min read
Aubreigh Lee Daculug
:
May 8, 2026
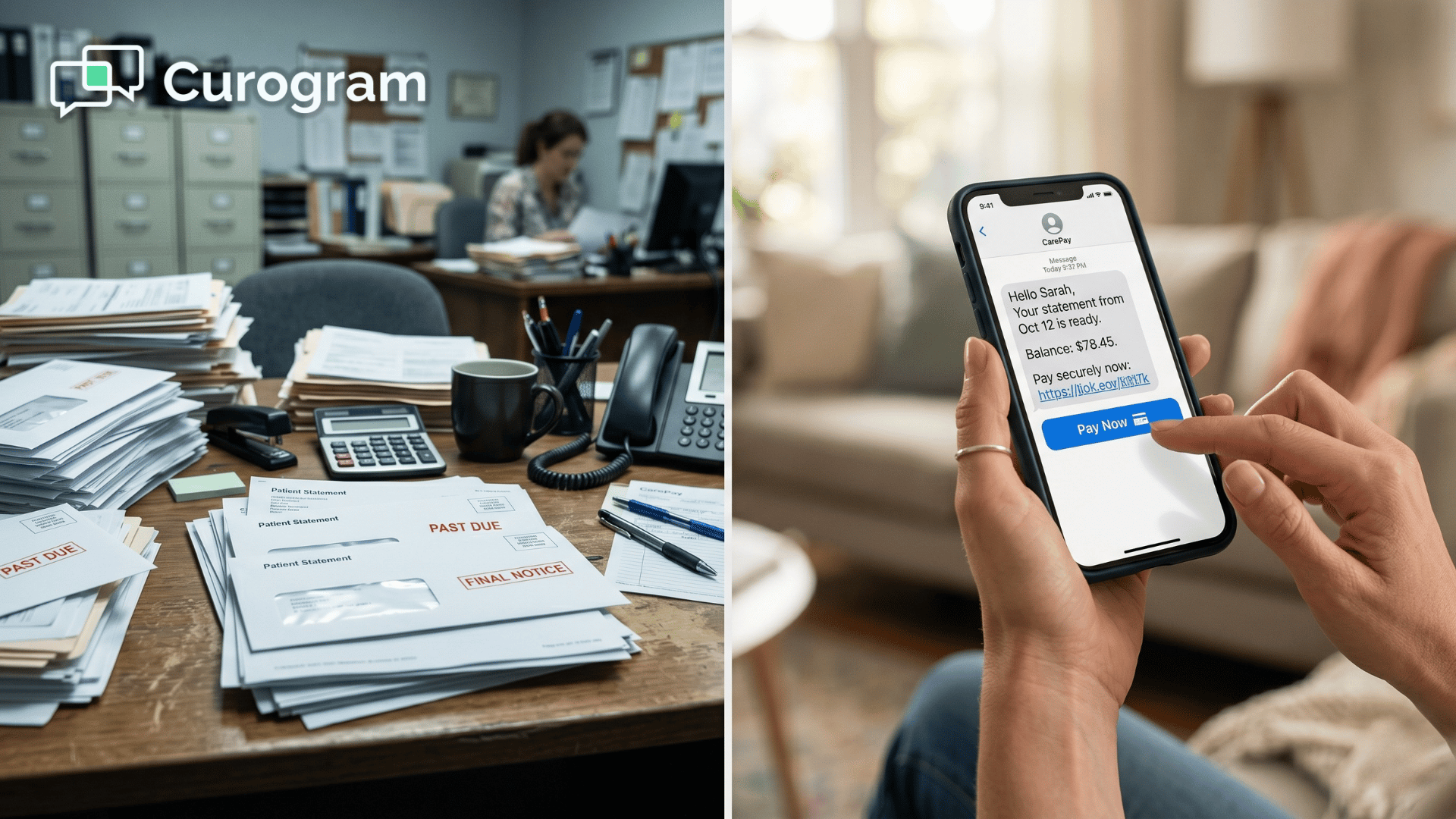
Picture this. Your revenue cycle team mailed 10,000 statements last month. Most were never opened. Some never arrived. A few sat in junk-mail piles for weeks.
By the time patients noticed them, your A/R aged another 30 days. That is the quiet cost most CFOs underestimate.
Paper statements feel safe. They look official. They cost a fortune.
For a 50-location enterprise health system, paper billing eats $40,000–$50,000 every month. That is $480,000–$600,000 a year on a medium that fails 80% of the time. The math does not work.
Now think about your own behavior. When did you last open a piece of mail within an hour? When did you last ignore a text? Patients are no different. They check texts 50 to 100 times a day. They open mail once a week, if you are lucky.
Your billing strategy is built for 1995. Your patients live in 2026.
This is where enterprise SMS payment collection text-to-pay for healthcare billing changes the equation. Instead of waiting weeks for a statement to land, a secure SMS reaches the patient in seconds.
Instead of a 17% conversion rate, you see 40–50%. Instead of staff chasing payments by phone, the payment closes itself.
The shift sounds small. It is not. It rewires the entire revenue cycle.
In this guide, you will see why paper billing keeps failing, how text-to-pay actually works inside an enterprise EHR like Oracle Health, and what the financial impact looks like when you model it across a 50-location system.
You will also see how Curogram handles HIPAA, PCI DSS, and SOC 2 Type II compliance so your CIO and compliance officer sign off without friction.
By the end, you will have a clear, numbers-backed view of what to do next.
Enterprise revenue cycle run on a model that no longer matches how patients pay. The economics, the behavior, and the staff workload all point in the same direction. Paper is failing.
Let's break down where the leaks are happening.
Every mailed statement carries hidden weight.
Most CFOs only count postage, but the full cost runs deeper:
Stacked together, these add up to $800–$1,000 per location each month. Multiply that across 50 locations and you are looking at $40,000–$50,000 a month, or $480,000–$600,000 a year, before a single dollar comes back.
Now layer in the conversion rates. The first statement converts at 15–20%. The second drops to 5–8%. The third? A painful 2–3%.
After three rounds, 70–80% of paper statements still have not generated a payment.
Here is what that looks like in practice.
A 50-location system with 50,000 patients and a $200 average statement volume sends out 10,000 monthly statements.
At 18% conversion, only 1,800 patients pay.
The cost per paid patient lands around $277. The remaining 8,200 sit in collections limbo, exposing the system to roughly $3,300 per uncollected account in bad debt risk.
You are spending the most money on the medium that fails the most.
SMS adoption is now above 95% across every age group, including seniors. Patients glance at their phones dozens of times a day. They do not glance at their mailboxes.
Mail itself is unreliable. Between delivery delays, forwarding gaps, and household mail piles, 10–15% of statements never reach the patient. Even when they arrive, they often disappear under junk mail.
Compare that with a text. It lands in seconds. It shows up on the lock screen. It gets opened in under a minute.
A patient knows they owe $200 within 30 seconds. If the payment link is one tap away, many pay before they put the phone down.
9,500 of 10,000 |
| SMS successfully delivered in a typical enterprise rollout, after accounting for disconnected numbers and opt-outs. |
When statements fail to reach patients, the work shifts to your team. Phone calls. Follow-up letters. Payment plans. Manual posting.
For 10,000 monthly statements, even a 2–3% phone contact rate generates 200–300 inbound calls. That eats up 1,000–2,000 staff hours every month.
The work is also miserable. Patients are confused (they never saw the bill), defensive (they didn't know they owed anything), and frustrated (they need options nobody explained). Your staff absorbs all of it.
This is why revenue cycle turnover stays high. Replacing one team member costs 30–50% of their annual salary. For a 5-FTE team at $50,000 average pay, a single departure costs $75,000–$125,000 once you factor in lost productivity and recruiting. The math compounds quickly.
The fix is not another portal. It is not another login. It is meeting patients where they already are.
Text-to-pay collapses the time, friction, and cost between billing and payment, aligning with broader revenue cycle process automation strategies.
Here is how it actually works inside an enterprise environment.

Curogram's text-to-pay platform connects directly to your Oracle Health billing system and pulls unpaid balances in real time. When a balance crosses a threshold you set, like 30 days past due, an SMS goes out automatically.
The message is simple:
"You have an outstanding balance of $250 from your visit on [date]. Pay securely: [link]."
The link opens a secure, one-time payment page. The patient sees the balance, picks a payment method (credit card, debit card, or ACH), and finishes the transaction in under 60 seconds. A confirmation text follows immediately, and the payment posts to your billing system within seconds.
No portal. No password. No EMR login. Just a tap and a payment.
That simplicity is why initial SMS outreach converts at 40–50%, two to three times the rate of paper.
4,275 patients |
| Tap the payment link out of every 10,000 statements sent, a click rate paper statements simply cannot match. |
Enterprise compliance teams ask three questions:
Where is the card data?
Where is the patient data?
Who is auditing this?
Curogram's text-to-pay is PCI DSS Level 1 compliant, which is the highest level of payment security.
Card data never touches Curogram's systems or your EMR. When a patient enters their card, the data flows directly to a PCI-certified processor like Stripe or Square through encrypted channels. Curogram only receives a payment token, never the card itself.
HIPAA protections layer on top. Patient phone numbers stay encrypted at rest. SMS transmission uses TLS 1.2+ encryption in transit. Payment links expire after a single use. Every transaction is audit-logged with timestamp, patient ID, amount, and status. A HIPAA Business Associate Agreement is standard.
SOC 2 Type II certification covers the rest, including access control, change management, and incident response. For your compliance team, that is the same level of assurance internal audit demands.
Integration is where most "innovative" tools fall apart. Curogram avoids that trap.
The platform connects to Oracle Health's billing module through an API. It reads phone numbers, outstanding balances, dates of service, and provider info. Payments flow back into Oracle Health's A/R module in real time, updating balances and payment history without manual entry.
Your revenue cycle team sees no workflow change. Payments captured by SMS appear in the same A/R dashboard, sorted the same way, exactly where staff already look.
For your IT team, the lift is light. Curogram's integration requirements are short and standard:
No VPN tunnel. No hardware install. No months-long implementation.
It is the kind of integration that gets approved in a single review cycle.

Here is where it gets interesting for your CFO. The conversion lift, the cash flow acceleration, and the operational savings all stack on top of each other.
Let's walk through the math.
Take a representative 50-location system with 10,000 monthly statement-eligible balances. After deploying text-to-pay, the first-touch conversion looks dramatically different from paper.
38% |
| Net first-touch payment conversion via SMS, compared to paper's 15–20%. |
Paper's number arrives 3–7 days later because of mail delays. SMS conversion happens within 24–48 hours.
Add a 7-day reminder and a 14-day final notice and overall conversion climbs to 45–50%, compared to paper's 20–25% after three full rounds. The full SMS cycle finishes in 14 days. Paper takes 21–28.
Faster, cheaper, and better. That is rare.
Payment velocity, the time from statement aging to actual cash receipt, is where the financial impact compounds. With paper, the average is 25–30 days. With SMS, it drops to 3–5 days.
3,800 patients paid |
| Out of 10,000 statements in a single billing cycle, all closed within days instead of weeks. |
Run the numbers on a system with $5M in annual statement-eligible balances. Cutting payment velocity from 27 days to 4 days adds about $1.5M in average daily cash on hand. At a 1–2% cost of capital, that is worth $100,000–$200,000 a year in working capital improvement.
Then add the conversion lift. Moving from 18% to 40% on $5M in balances brings in $150,000–$250,000 in incremental collections.
Now stack the savings from eliminating paper, $480,000–$600,000 a year. The total year-one financial impact lands between $630,000 and $1,050,000 for a single mid-sized enterprise system.
That is not a software upgrade. That is a margin expansion.
Bad debt write-offs track closely with reach. If 70% of patients never see a bill, those accounts are headed for write-off whether you like it or not. Push reach to 95% with SMS and the math changes.
Health systems using text-to-pay typically see a 20–30% reduction in bad debt write-offs. On a 1% baseline write-off rate against $5M in balances ($50,000 per year), that drop saves $10,000–$15,000 annually. Larger systems scale the savings linearly.
The staff impact is bigger than most CFOs expect. Revenue cycle teams spend 40–60% less time on phone-based collections once SMS handles outreach.
A 5-FTE team can redeploy 2–3 FTEs to higher-value work:
Or trim headcount entirely and save $130,000–$225,000 a year.
For your team, this means fewer angry calls, less burnout, and more time on work that actually moves the financial needle.
Paper statements are not just expensive. They are the slowest, lowest-converting part of your revenue cycle. Every month you keep them, you lose money on the front end and cash flow on the back end.
Text-to-pay does not require a system overhaul. It plugs into Oracle Health, respects your compliance stack, and starts producing results in the first billing cycle.
Your patients pay faster. Your staff stops chasing. Your CFO sees the numbers move.
The financial story is consistent across every enterprise deployment.
A 50-location system can recover $600,000 to over $1 million in year one through a combination of paper elimination, conversion lift, accelerated payment velocity, and reduced bad debt. Add staff redeployment and the impact deepens.
The compliance story is just as clean. PCI DSS Level 1 keeps card data out of your environment entirely. HIPAA protections, BAA coverage, and SOC 2 Type II certification handle the rest. Your security and compliance teams get every audit artifact they need.
The implementation story is the easiest part. OAuth authentication, REST APIs, outbound HTTPS only. No VPN, no hardware, no painful onboarding.
Most enterprise health systems are sending their first text-to-pay messages within weeks, not quarters.
So here is the next step. Book a 15–20 minute walkthrough with the Curogram team. You will see the text-to-pay interface, the secure payment link experience, the Oracle Health integration in action, and a live look at the dashboards your revenue cycle team will use every day.
Bring your A/R numbers. We will model the financial impact against your real volume, your real conversion rates, and your real paper costs. No assumptions. No fluff.
Schedule a demo today and see exactly what enterprise SMS payment collection text-to-pay for healthcare billing can deliver inside your system. The first cycle will tell you everything you need to know.
Text-to-pay links are secure because they never expose patient data and never store payment information. When a patient taps a Curogram text-to-pay link, they are routed to a secure, one-time-use payment page operated by a PCI DSS Level 1 payment processor. Their card data flows directly to that processor over TLS 1.2+ encryption. Curogram and your EMR never see the card itself. The processor returns only a payment token, which is logged against the patient account. PCI DSS Level 1 compliance means the processor has passed rigorous third-party audits of every payment security control, so card data stays out of your healthcare environment entirely.
Curogram's platform includes automated fallback. If an SMS bounces because of a disconnected number, the account gets flagged and routed to an alternative outreach method like email, paper, or an automated phone call, based on your configuration. For patients who opt out of SMS, Curogram respects the preference and routes them through your default collection channel. This hybrid approach keeps you reaching 95%+ of your patient base while staying aligned with patient preferences and regulations like TCPA and state privacy laws.
Text-to-pay links can route patients to a simple payment plan intake form where they enter what they can afford and how often they can pay. That form ties directly into your revenue cycle system's payment plan module, so plans can generate automatically based on patient input. Links can also include a callback request for your financial counseling team. The goal is to give patients real options inside the SMS itself, which lowers friction, lifts conversion, and reduces repeat outreach. Patients who cannot pay right away get contacted once instead of repeatedly, which improves satisfaction and cuts call center volume.
Most enterprise health systems are live with text-to-pay within 4–8 weeks, not quarters. The integration uses standard REST APIs and OAuth authentication, so there is no VPN setup, no hardware install, and no shared credentials. Your IT team only needs to allow outbound HTTPS traffic on port 443. The bulk of the timeline goes to mapping your Oracle Health billing fields, configuring SMS triggers (like the 30-day past-due threshold), and running compliance review with your security team. Curogram provides BAA documentation, SOC 2 Type II reports, and PCI DSS attestations up front, which usually accelerates the review process. Once configured, you can roll out by location, by department, or all at once.
Yes, and the data on this surprises most CFOs. SMS adoption is now above 95% across every age group, including patients over 65. Older patients may not use apps or portals, but they almost universally read text messages. The text-to-pay link works on any phone with a basic web browser, including older smartphones. For the small percentage of patients without SMS access, Curogram's automated fallback routes them to your default channel, whether that is paper, email, or phone outreach. You do not lose reach with older demographics. In many enterprise deployments, patients aged 55+ actually convert at higher rates than younger patients because they tend to act on bills more quickly once they see them.
💡 SMS payment collection revenue cycle ROI healthcare improves three numbers fast: payment conversion, days-in-A/R, and bad debt. Paper statements...

💡 RamSoft imaging center text-to-pay is a secure, SMS-based patient payment system that collects copays, deductibles, and coinsurance directly...
💡 Text-to-Pay for GE Centricity helps multi-location specialty and radiology clinics accelerate patient payment collection through automated SMS...